Lyme Vaccines Show New Promise, and Face Old Challenges
Jessica Reeder worries about ticks and the diseases they carry. She had Lyme disease, her brother had Lyme disease, and every fall her children come home from school with notes reminding parents to do a nightly tick check. Even in Philadelphia, where Reeder lives, the bloodsuckers lurk in the woods around the playground. Her family used to go tent camping with friends, but they stopped after a few people in the group contracted Lyme.
“It just got to the point where people were too stressed out about it,” she says.
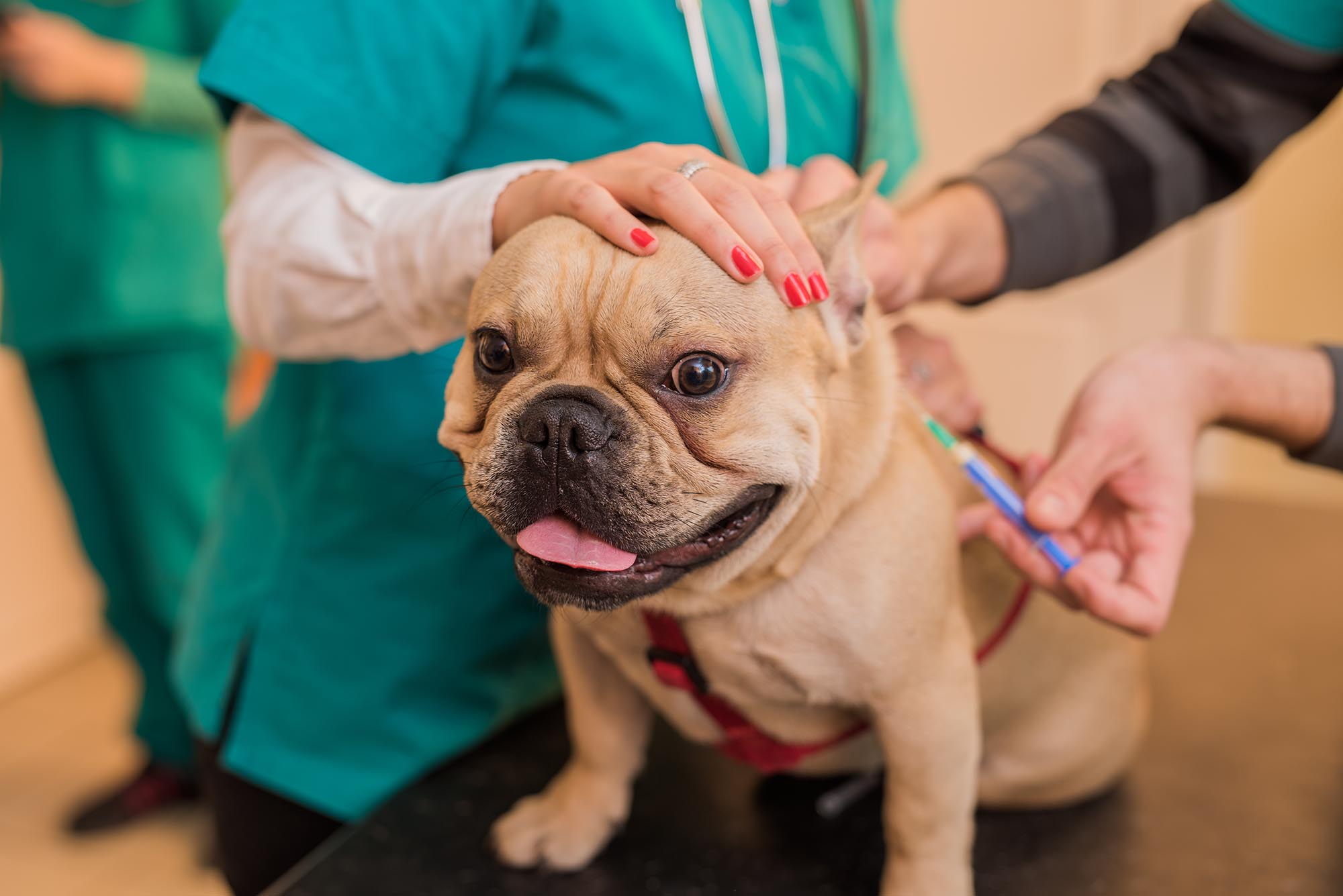
Reeder made sure her Shih Tzu, Rory, got the canine Lyme vaccine, but must protect the human members of her family the old-fashioned way: bug spray, long pants tucked into socks, and frequent tick checks. There’s no Lyme vaccine on the market for humans.
Valneva, a French biotech company focused on developing vaccines for infectious diseases, hopes to change that. Six years ago the company began working on a vaccine against Lyme disease, which is now part of phase II clinical trials in the United States and Europe.
A safe and effective Lyme vaccine would be a boon for public health. According to the Centers for Disease Control and Prevention (CDC), hundreds of thousands of people are likely diagnosed with Lyme annually in the U.S. Tens of thousands more develop Lyme each year in Europe. Caught early, the disease is usually easy to treat. But not every infected individual displays the hallmark symptom of Lyme — a bull’s-eye rash — and so the disease sometimes goes undetected. Left untreated, the bacteria can cause severe joint and nerve pain, memory problems, dizziness, and heart palpitations.
Valneva’s Lyme vaccine isn’t the first designed for people. Twenty years ago, Reeder could have been immunized. From 1999 to 2002, SmithKline Beecham — now GlaxoSmithKline — sold a Lyme vaccine called LYMErix. But the company pulled LYMErix off the market after a public backlash and a spate of lawsuits.
As STAT reported on August 22, any new Lyme vaccine will face intense public scrutiny. But even getting the new vaccine to market could prove challenging. Valneva is currently seeking a partner to help develop and commercialize the vaccine, and at least one major manufacturer is out of the running. GlaxoSmithKline had been supporting the new vaccine’s research and development, but in June the two companies terminated their partnership.
If the new vaccine does make it to market, will it fare any better than LYMErix? According to Gregory Poland, co-director of the Vaccine Research Group at the Mayo Clinic in Rochester, Minnesota, who has given scientific advice to Valneva, that’s “a multi-million dollar question.”
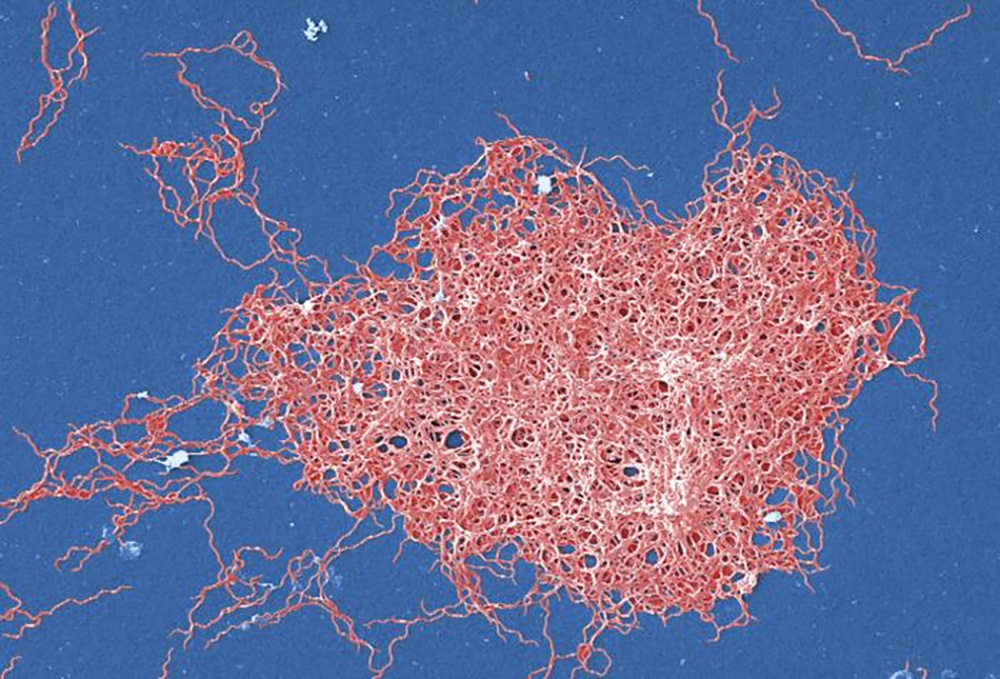
One factor that led to LYMErix’s demise hinged on how the vaccine worked. Lyme disease, named for the Connecticut town in which it was first discovered, is caused by a corkscrew-shaped bacterium called Borrelia burgdorferi that travels in the bellies of ticks. LYMErix prompted the immune system to generate antibodies against a protein on the surface of the bacteria called outer surface protein A (OspA). When a tick fed on someone who had been immunized, it ingested blood containing the Lyme-killing antibodies. Those antibodies traveled to the tick’s gut and wiped out the bacteria before it could enter the human body.
LYMERix worked, although imperfectly. A 1998 study in the New England Journal of Medicine looked at nearly 11,000 people who lived in Lyme-endemic areas and found that those who received three doses of LYMERix had a 76 percent reduction in Lyme disease the following year compared with those who didn’t receive the vaccine. But just a week after the study was published, another paper came out showing that one particular portion of the OspA gene bears a striking resemblance to a portion of a human gene that plays a role in the body’s immune response. While the second paper didn’t address vaccination, the researchers posited that, because of the similarity, some people infected with Lyme disease might develop an immune response against the human protein, leading to lingering inflammation and treatment-resistant Lyme arthritis. But it wasn’t a stretch to imagine that vaccination, which also prompts an immune response against OspA, might produce the same effect.
The Food and Drug Administration never found any compelling scientific evidence to support this theory, but that didn’t stop people who believed they were harmed by the vaccine from speaking out and filing a class-action lawsuit. Sales of LYMErix tanked, and in 2002 SmithKline Beecham withdrew the vaccine. The following year, the company paid more than a million dollars in legal fees to settle the class action lawsuit.
The withdrawal of the vaccine had a chilling effect on the entire field, says Maria Gomes-Solecki, a veterinarian at the University of Tennessee. In the late 1990s, when LYMErix was first approved, she was working on developing a new and improved OspA vaccine. But when SmithKline Beecham pulled LYMErix off the market, Lyme vaccine research “basically went dead,” she says. “No one wanted to touch it.” Even Gomes-Solecki decided to go in a new direction. She repurposed her work into an oral vaccine for mice (one of the main reservoirs for Lyme disease). The Memphis-based company U.S. Biologic is now seeking approval from the U.S. Department of Agriculture to market the mouse vaccine, which would be delivered in pellets of food set out as bait.
SmithKline Beecham wasn’t the only company to pursue a human Lyme vaccine. Pasteur Mérieux Connaught (now Sanofi Pasteur) developed an OspA Lyme vaccine called ImuLyme and tested it in a large efficacy study. The ImuLyme results came out in the same July 1998 issue of the New England Journal of Medicine as the LYMErix results. But the company never applied for a license to market the vaccine.
More than a decade later, the pharmaceutical giant Baxter also tried developing a Lyme vaccine. The company completed a safety study in 2013, but despite promising results, never launched a follow-up. Today Takeda, the largest drug company in Asia, owns that vaccine and is evaluating whether to take it forward.
“Every manufacturer that has considered this since 2002 has judged that it’s unlikely that we’re going to make a profit on this vaccine,” Poland says. “In the second decade of the 21st century, you can protect your dog against Lyme disease, but not your children.”
There are signs, however, that the field is beginning to warm to a human Lyme vaccine. In December 2016, Congress established the Tick-Borne Disease Working Group to help identify research priorities. The diverse, 14-member working group within the Department of Health and Human Services includes researchers, physicians, patients and their family members, patient advocates, and employees from a variety of federal agencies. Last December, the group released its first report to Congress, calling for increased federal funding to address the “serious and growing threat” of tick-borne diseases.
In April, the National Institutes of Health (NIH) announced that it intends to commit $6 million in fiscal year 2020 to more than a dozen projects aimed at the prevention of tick-borne diseases, including vaccine research.
Meanwhile, Valneva is conducting its phase II clinical trial in the U.S. to determine the final dose and vaccination schedule. The company should have the initial data by the middle of 2020. The next step will be to launch two efficacy trials including about 8,000 people each, one in Europe and one in the U.S. The company could seek regulatory approval in about five years.
Valneva’s new vaccine works like LYMErix, but with two key differences. LYMErix only provided protection against one strain of Borrelia found in North America, while Valneva’s vaccine protects against the six most common strains in the northern hemisphere, including those in Europe. Also, Valneva has eliminated the human protein-mimicking segment of the OspA protein and replaced it with a similar sequence from another strain as a “precautionary measure,” says Thomas Lingelbach, Valneva’s CEO. The company doesn’t have human efficacy data yet, but Lingelbach doesn’t expect that the swap will affect the vaccine’s ability to protect against the disease.
Demand for a Lyme vaccine should be greater than ever before. When LYMErix first hit the market in 1998, the number of reported cases was about 17,000. By 2017, that number had climbed to roughly 30,000 confirmed cases. And the CDC estimates that far more — some 300,000 people — are actually diagnosed each year. “In the ‘90s, Lyme disease sounded like some exotic thing that happened elsewhere,” Poland says. Today, especially in regions where Lyme disease is endemic, almost everyone knows someone who has been infected. The number of people who contract Lyme disease in Europe is harder to pin down, but some estimates point to as many as 200,000 cases each year.
And because the problem has grown, the medical experts who develop recommendations on how to use vaccines — the Advisory Committee on Immunization Practices in the U.S. — might look more favorably on a Lyme vaccine, says Stanley Plotkin, a physician and emeritus professor at the University of Pennsylvania. The committee gave LYMErix a tepid recommendation back in 1999. Even for adults in the highest risk group, it stopped short of a full endorsement. That likely wouldn’t happen today, Plotkin says, because “the need for a vaccine, both in Europe and the U.S., is manifest.”
While anti-vaccine sentiment is still a problem today, as evidenced by the increasing number of measles cases in the U.S., “I think the tide has begun to change,” Poland says. Lise Nigrovic, a pediatrician and emergency room physician at Boston Children’s Hospital and a former member of the Tick-Borne Disease Working Group, argues that unlike with a disease such as measles, which spreads quickly from person to person and where ensuring high vaccination rates becomes crucial to maintaining herd immunity, Lyme vaccination is more of an individual choice and less likely to be an anti-vaccination target.
But Valneva can’t bring the vaccine to market without a commercial partner. “The ideal partner will have deep experience in developing and commercializing vaccines, as well as an in-depth understanding of Lyme disease,” Lingelbach says. But finding that partner could prove challenging.
When GlaxoSmithKline terminated its partnership with Valneva in June, that put one of the five top-earning vaccine makers out of the running. Only one of the remaining four, Merck, confirms it is working on a Lyme vaccine. “Our researchers involved in early discovery are looking at the space,” said Pamela Eisele, global communications director at Merck, by email. Neither Pfizer nor Novovax has a Lyme vaccine in development. And Sanofi Pasteur did not respond to repeated requests for comment.
Convincing the public to get immunized could also prove challenging. Valneva has yet to determine the number of vaccine doses, and when those doses must be administered. But Lingelbach anticipates people will need three shots over the first two to six months, a booster after a year, and then additional boosters perhaps every three years. That’s inconvenient, especially for adults who don’t visit the doctor regularly.
There’s also the perception of safety. “Vaccines have this really high bar because they’re given to healthy people who don’t have a disease,” Nigrovic says. “So even just the hint of a problem, it makes people really nervous,” even if there’s no evidence the problem is linked to the vaccine.
The controversy around LYMErix has faded from the public’s awareness. “Time has done some healing,” says Richard Marconi, a microbiologist at Virginia Commonwealth University. But the report from the Tick-Borne Disease Working Group also makes it clear that the perceived damage inflicted by LYMErix has not been entirely forgotten. One of the group’s recommendations was to support the development of safe and effective human Lyme vaccines. But in a dissenting minority response, the authors write: “the search for a new vaccine should only commence when the science behind the past vaccine failure is understood.”
Among Lyme advocates and the chronic Lyme community especially, skepticism about a Lyme vaccine persists. According to Patricia Smith, author of the minority response and president of the Lyme Disease Association, a patient advocacy group based in New Jersey that has funded research on chronic Lyme and co-funded a center at Columbia University dedicated to studying the condition, the LYMErix situation was “very troubling.”
“Certainly we’re not averse to vaccines,” Smith says, but she’s frustrated that little effort went into finding an explanation for why so many people reported ill health effects from LYMErix. Smith does not find Valneva’s decision to remove the controversial portion of OspA from the new vaccine all that reassuring because it was never clear that piece of the protein was to blame for the symptoms people reported. “We’re very concerned by it,” she says. “We don’t know what is going to happen with this one.”
Because of LYMErix’s troubled past, Marconi still argues that avoiding OspA might be the best strategy for new vaccines. He has spoken with a handful of vaccine manufacturers and says the companies are wary about the backlash that could accompany another OspA vaccine. (He did not provide the company names to Undark, citing confidentiality agreements.) Marconi helped develop a canine vaccine, and is now working on a human vaccine that would target two other Borrelia proteins. But Plotkin says some companies might find an OspA vaccine attractive because they already know the approach can protect against the disease. “The probability of an OspA vaccine working is very high and that reduces the risk for manufacturers,” he says.
Lingelbach hopes that opening a direct line of communication between Valneva and the Lyme advocacy groups will help dispel concerns about OspA. “We are in contact with many key opinion leaders and plan to take a more proactive approach,” he says. “We encourage patients and advocacy groups to reach out to us and we’ll work with them to establish a dialogue.”
Reeder, however, doesn’t need much convincing. She wants her kids to be protected without having to dose them in DEET every day. If a new vaccine becomes available, she says, “we definitely would look into it.”
Cassandra Willyard is a freelance journalist based in Madison, Wisconsin. She has written for The New York Times, Discover, Popular Science, Scientific American, Nature, and many other publications.











Comments are automatically closed one year after article publication. Archived comments are below.
I have been in treatment for chronic Lyme for 7 weeks now with huge improvements. It is S5 herbal formula purchased from (ww w. besthealthherbalcentre. c om) that go after to wee beasties the biofilm and are switched up so the wee beasties don’t get resistant to it. The treatment also rebuilds your immune system and balances your body after being sucked dry. I had Lyme since late 80s and was close to death when I started on this treatment which includes massage. You need a qualified practitioner to take you through as each person is different and so the formulas are created for you. I have my sleep cycle back and wake up rested and fall asleep easily. That one is huge. My guts have settled down, they were a mess. Pain is much less brain fog way less just so much better all around. You do herx and it is not easy at first but over time things fall into place and better sleep becomes cumulative. It is a 8 to 10 weeks treatment but gets better as it goes.
Guys, people, PLEASE STOP preaching and teaching about the “bulls eye” rash trade-mark created by a tick. Please. Stop. I had a rash that was circular, about nickel-quarter coin size, but it was NOT bulls eye shape nor, again, was it a complete circle. Because of this, I thought I had some skin abnormality or deformation developed and that it might go away. Later, I had a doctor see it and they didn’t think much of it also. I now STINKING SUFFER the damages created and left by that disease. STOP YOUR “bulls-eye” tradition and generalized teaching of the rash created by ticks. Please start using “Circular” instead, the size of a “nickel” or “quarter”-“generally.” You must use these basic, general, but maybe Life-Saving terms instead of the bulls eye term. Please. Thank you.
While a Lyme vaccine would be ideal, I would like to point out that you can heal yourself of Lyme and all of its confections using a quality Rife machine. I healed myself of 25 years of Lyme this way and then started a group in which I met a local doctor who healed his near terminal Lyme the same way.
I had a client in Baltimore who was suffering and I kept trying to get him to buy a Rife machine but he had one of the top Lyme docs in the country and trusted him. Only after a year of hassling him did he finally ask this very famous doctor. The docs face lit up and he said that he had cured HIS OWN LYME with a Rife machine, but did not dare mention it until his patient mentioned it first……If you want to read of a real tragedy and travesty, read Barry Lines [not Lymes!] book, The Cancer Cure That Worked.
Big Pharma has been repressing the best medicine for our major diseases forever. Their principal goal is not curing us but is making money. But so many people love their doctors….It is not the doctors, it is the system. The triad of allowable treatments- surgery, chemo and radiation, miss the diamond of medicine, which is frequency medicine. Try not to comment if you are ignorant of Frequency medicine and just want to repeat the lies of Big Pharma. I have watched numerous friends die of Lyme, and have watched as the ones who used Rife machines just continually get better. Get Brian Rosner’s book, Lyme Disease and Rife Machines.
I was one of those people permanently injured by the Lymerix vaccine. In the late 90s I was doing a lot of field work and often found myself covered in ticks. I got the first two shots about three weeks apart. I never went back for the third shot because within a few days of the second shot, I got severe stiffness in my extremities – hands, wrists, elbows, ankles, knees. If I spoke on the phone for a while (the old corded phones), I wasn’t able to straighten my arm to hang the phone up on its cradle on the wall. Walking to the bathroom when I first got out of bed in the morning was extremely difficult because I couldn’t bend my ankles. I never knew about the lawsuit or that the vaccine was withdrawn. I saw my doctor who never reported my symptoms. She sent me to a rheumatologist who told me he thought I was trying to get into a lawsuit. I wasn’t and I never did participate in a lawsuit. Over the years I’ve found very little info on the Lymerix vaccine except opinionators stating that it had to be pulled because so many people created symptoms so that they could sue the manufacturer. My symptoms were real. I still suffer all these years later. I once read an article that did say that most people impacted by the vaccine first got the symptoms after the second shot (as I did) and that the resulting stiffness mostly occured in the extremities, as it did for me. I really wish there had been more research into the impact of the Lymerix vaccine. We were dismissed as lawsuit hungry, rather than for the actual damage done by the vaccine. I’m not anti-vaccine. My children and my dog are all up to date on their vaccines. I’m a microbiologist by training. Something happened here that should have been properly investigated and never was. I hope the same doesn’t happen with a new vaccine.
Having chronic Lyme for 7 years has prompted me to self educate on the matter. Here is one very important warning for tick bite victims: the likely treatment
of a few weeks Doxycycline WILL NOT WORK IF CALCIUM (milk, cheese, yogurt, calcium antacids, or calcium supplements, etc.) is consumed surrounding the Doxy because the Doxy binds to calcium and becomes useless.Perhaps this is a large portion of the chronic Lyme epidemic because it is generally not stressed
with the prescription instructiobns.
Please see a court case about this:
https://www.baltimoresun.com/news/bs-xpm-2003-05-30-0305300377-story.html
Having previously caught lyme disease, I took LYMErix when it came out. It was my understanding that in addition to some people (not me) reporting serious side effects, the vaccine’s immunity lasted only a year. The latter was also a reason why the manufacturer pulled the vaccine.
I had a weekend house in rural Columbia county north of NYC in the 1990s. Our dog would often come home with what looked like a blister, or a growth. It was an engorged tick, that I learned how to remove. .
One day I noticed a red circle on my leg, maybe six inches in diameter. I called my N.Y.C doctor. I wanted to have a blood test but he demanded I take action immediately, so phoned the antibiotic to the local pharmacist. He was a caustic doctor who I never liked, but to this day I appreciate his no BS response that may have saved me from a chronic problem. BTW, I did get the first shot of the vaccine, before they withdrew it.
Now I live in a boring suburb of San Diego, but while I do have to worry about earthquakes and fires, we don’t have lime disease-yet
This is a comment about the Lyme vaccine for dogs. I had my young, healthy retriever-mix vaccinated for Lyme. I didn’t realize that Golden and Labrador Retrievers seem to be predisposed to developing Lyme nephritis, a kidney disease which is usually fatal. Within a few days after getting the vaccine, my dog went into kidney failure and died. I later learned that due to this predisposition some retrievers can get nephritis as an adverse reaction to the Lyme vaccine itself, so I would urge caution if you have a retriever and are considering the vaccine.
Using the conspiracy garbage site whale.to as part of your argument automatically negates everything you’ve claimed.
Considering Lyne disease is a bioweapon first developed on Plum Island by the US military in the 1950s, thanks to the tech they got from the nazi scientists they brought to the US under operation paperclip, a vaccine against lyme would be more of the same. Why not simply treat against the toxins that are in Lyne disease, such as mycoplasma, parasites, and viruses, most of which could be treated with an anti-parasitic like diatomaceous earth, anti-fungals like apple cider vinegar, and anti-viral treatments which are present in many essential oils like rosemary, thyme, tea tree, and oregano.
It is time the real truth about Lyme disease and other bioweapons released on the American public and global populace by an out of control DOD and research community was made public.
I hope your tinfoil hat is firmly in place, to protect you against those brain waves the CIA is shooting out from the chemtrail planes.
Wow. The depth of ignorance in this comment is staggering. First, mycoplasm, parasites and viruses are not toxins. They are living organisms. Mycoplasmas are a group of bacteria that cause several different diseases, none related in any way to Lyme. Parasites could be intestinal worms, heartworms, blood parasites such as some protozoa–again, no relation whatsoever to Lyme disease. Viruses have no connection whatsoever to Lyme. It’s caused by a totally different organism, a spirochetal bacterium. Moreover, Borrelia (the bacterium that causes Lyme) does not produce toxins itself, such as some other bacteria do.
If you seriously think that Lyme disease can be cured with diatomaceous earth, apple cider vinegar,rosemary, tea tree [oil] or oregano, then I’d like to invite you to expose yourself to Lyme and then document how you cured your infection. You’ll have the attention of the entire world if you can do that, I promise you.
His/her use use of “toxins” may have been misused: they probably meant toxins in the effect that it is harmful to/for humans. One must be reasonable when reading someone’s comments (and researching) because interpretation and perspective can have a large gap with anyone else’s if we don’t check our senses. Age, gender, the way one was raised, where one was raised, their conditions or environment, and more, must be considered if we are to understand someone else’s actual wording. More so, it is a fact that hospitals and pharmaceuticals are affiliated in treating others and that money is all that matters in the end. Saying natural remedies are what the world is waiting for by way of “researchers” is saying you don’t care for such remedies but that you will trust “science” until they say any given natural resource or treatment works, and that will NEVER happen. Why don’t use the heart of a apricot seed to treat (maybe not cure) cancer? It is a well established fact that it works. “Scientists” working for the Huge tobacco industry use to say tobacco didn’t have any addictive substance, too, but now we know it does. It’s always, and always will be, about money first and foremost. Some science(s) are great and amazing, but many come VERY short on helping the human race achieve great health and prosper.
Lyme disease was discovered in the 5,000 year old Oetsi frozen body in Switzerland (watch the several NOVA PBS shows) which contributed to his arthritis problems. The DOD hasn’t been around that long. It was brought from Europe to the New World with the colonist and their rats.
But that was not Lyme disease. They WANT it to be Lyme so, like some other “sciences,” they push the IDEA that it was Lyme.
The main problem here which no one is talking about is the increase of ticks throughout many areas of the country. It’s a huge problem and getting worse year over year. There are too many deer and maybe too many other critters carrying the ticks without a population of predators. So, an animal sick from a tick bite lives a much longer life allowing for the spread of whatever disease it’s carrying over a longer time span. And yes there are more tick diseases than lyme. If you live in a city you probably don’t give a whoot about what’s going on. Until of course when one of your children comes home from summer camp with a disease which may affect them the rest of their life. We need more money put into finding good vaccines even if they are only partially effective AND we need to find a way to drastically lower the population of all ticks. Might not be easy but this thing is going to bite us all in the posterior if we don’t recognize the extent of the problem we already have.
Actually, it is not deer who are the greatest hosts for the ticks. It is mice and other small animals. ………https://www.wideopenspaces.com/know-opossums-eat-virtually-ticks-yard/
Living in an area (Southern VT) that has seen the influx of TBD (tick borne diseases) from virtually nothing to endemic over the past 25+ years I would urge folks to pay particular attention to your comment regarding mice and other smaller vectors. Certainly deer, birds and other warm blooded creatures are also known to be hosts.
One of the ways we humans can impact this cycle is the use of either commercial or homemade “tick tubes”. These tubes are filled with permethrin treated cotton batting and distributed for mice to take from as bedding for their nests, thereby treating that family to a tick-killing lair.
I’d also offer this observation and my own theory; the increase in Fox population in our area has lead to a very noticeable DEcrease in squirrel and chipmunk numbers. I do believe Mother Nature can and does play an important part in offering some controls, much in the same way as a severe winter will cut down on deer herd populations.
YES the increase in ticks due to climate change. The ticks and their hosts are not being killed off during the deep freezes of winter, and the season for reproduction is longer.
I have read this article and a couple things come to mind. As a Microbiologist prior to attending Med. School, I have some expertise and understanding at the level of the microbiology put forth. As a physician, I look at things with a slightly different perspective. The issue of the vaccine not treating all strains of the Borrelia sp. is not likely known (positive or negative). As one of the commentors explained the ILADS Group has identified a series of different organisms that cause similar symptoms (sxs) but would NOT be covered with as specific a vaccine as proposed and are NOT treated with the same form of treatment, e.g., Babesia would best respond to Metronidazole which would NOT treat Borrelia, etc. The “Anti-vaccine” group seems to offer an argument that making the choice to NOT vaccinate endangers an unsuspecting group when it only really endangers those NOT vaccinated and that was a choice that the responsible party for those children need to address. The rest of the population can be vaccinated by CHOICE and should not be at risk. Whether this is the most appropriate approach is up for discussion and decision making. To sum this up, why not work against the known understanding that much is NOT known and issues may occur that look like mistakes but really may only be a reflection of the Newness and current Lack of Knowledge in this area. After all, Louis Pasteur was considered a charlatan by his contemporaries until van Leeuwenhoek came up with a device for looking at the micro organisms that Louis described. Koch came along with a series of Postulates that would establish a “cause and effect” relationship to seal the deal. We need to move ahead in some fashion as there are a huge number of people that are effected by a “complex” pathogenic system and the desire to look at it “too close to determine what we see” or ignore it because of adverse outcome is not in the patient’s best interest. Add to this part of the issue the CDC’s reliance on a set of diagnostic criteria that guarantees a huge series of “False Negatives”, we need to be more aggressive in this area.
Your observation that “Louis Pasteur was considered a charlatan by his contemporaries until van Leeuwenhoek came up with a device for looking at the micro organisms that Louis described.” has one problem: van Leeuwenhoek died in 1723, 99 years before Pasteur was born. Pasteur was well aware of microorganisms, as were his contemporaries. Pasteur’s contributions included proving that microorganisms reproduced and were not generated spontaneously and showing that weakened microorganisms, used as a vaccine, could provide specific protection against disease caused by a more robust form of the same microbe.
Agree ,false negatives needs to be main issue to catch in time to treat ….OR ….just treat it can’t hurt !
I moved to the country in 1999, I asked my doctor for the Lyme vaccine and he told me not to bother with it. 1) it’s expensive. 2) you need multiple shots. 3) Lyme disease can be tested for. 4) If you get it it can be cured. So I never got the vaccine.
Your doctor is like most doctors on the subject of Lyme. A complete and utter idiot.
i agree about the doctors that ignore, lie and walk away from sick people. i have seen them all. They are worse than idiots. They are living a lie. They know that these lyme sick people are handicapped in mental and physical terms, and yet they ignore them. i have even had a doctor raise his voice at me for helping another ill person. Healthcare is not to help others anymore. It is for making money. Yes, I would like to hear in laymens terms, why the lyme vaccine did not work. also, I’d like to hear why the CDC changed the definition of lyme on the lyme tests, leaving out approx. 85% of the people sick with lyme in 1992.
The LIMErix vaccine contains 500ug of aluminum adjuvant, as much as Gardasil 9. Gardasil 9 causes more injuries than any other vaccine. It’s entirely possible that the injuries caused by LIMErix are due to its direct neurotoxicity, not to induced auto-immune illness. For more info on aluminum toxicity in vaccines, see vaccinepapers.org (complete with full-text copies of the peer-reviewed research it cites).
Oh, the old “aluminium” issue again? Shake your head! In the US you now have an outbreak of measles, because your “ilk” has been trying to convince everyone that inoculations of any type are bad!
Additionally, and not pertaining to your comments: The issue of Lyme Disease has been totally blown out of reality! 30,000 diagnosed cases in 2017??? So what?? More people expire from squeezing a zit! I have had the classic “bulls eye” twice, and a third time without the sign, but the tick was right there on my scrotum, had to have my better half take a picture of it so I could see it! The female Doctor literally shrieked (I took it in in an empty pill bottle) then she had to get on the phone for half an hour to find out that I needed one antibiotic tablet! We stopped on the way home, at the local Veterinarian, he dumped it out on the counter and said: “Yep, that’s a black-legged deer tick.” After my first encounter, my Doctor put me on Minocycline, (a type of tetracycline) for a year, many years ago. All hype (Lyme Disease) verging on mental instability!
I personally was permanently crippled by a series of vaccines. The one common ingredient in all of them was aluminum. But i am unable to find out the hard way! From now on, I have absolutely no faith in any vaccine. I am more frightened of the vaccines that I am all of the disease.
Now all the naysayers have to also recognize that Lyme disease is only one section of the nasty tick bite. There is a second hidden virus/bacterium involved that closely mimics Lyme. That has only recently been discovered ( within the last 3 years) and was totally unknown in the 2002 and before era. Symptoms & effects are similar. I remember that a blood test for Lyme back then was only about 50% accurate as well, and getting a doc to prescribe same was like pulling teeth. A year ago I lost a friend to complication’s of Lyme.
why don,t health insurer believe that lyme desease is a desease?
I got the vaccine in 2000, worked in deer tick habitat for years without getting infected. Maybe I was just lucky, but the vaccine seemed effective to me, and I’m certainly better off than my colleagues who got Lyme.
they did this to hiv victims too. said it didn’t exist till they came up with vaccine. tens of thousands are suffering in the dark right now with diagnosis but denial from a committee that decides how they will define a disease based on a failed vaccine that hurt a lot of people in experimental phase. its cover up cover up until a multimillion dollar market/pantent can be pulled from the pocket. they see a market, the american people, but will not allow the diagnosis and cure for those who have suffered for years if not decades. its a travesty.
Laura, what are you talking about. There is no vaccine currently or previously available for HIV. Some are entering human trial phases now and there have been tremendous advances in medication to treat and prevent.
Do you mean people who were part of a trial became ill or were denied other treatment while in the trial?
Jane, your argument–“Lymerix did not work without bad side effects, therefore no Lyme disease vaccine will ever work” is illogical to the extreme. And all your statements following that opening salvo in your post go to the safety/efficacy of Lymerix, and nothing else.
The article clearly discusses how the current vaccine being studied works differently than Lymerix and “protects against the six most common strains in the northern hemisphere, including those in Europe.” There are more than 300 strains of Lyme? Great–if the current vaccine being studied knocks out the six most common strains, then someone else can start tackling some of those other strains.
Maybe the new vaccine will be great, and maybe it won’t be. That’s what clinical studies are designed to suss out. If this one doesn’t work, I hope scientists will continue to look for a safe and efficacious vaccine. Arguing that no one should ever try to develop a vaccine to prevent a disease to which millions of people are susceptible is just ludicrous.
If lyme disease is a parasitic bacteria, like syphilis, how can they make a vaccine? Are there other vaccines for parasitic bacterial infections?
It’s not correct to say almost everyone knows someone who has been infected. The fact is, almost everyone has been infected, many of us more than once.
Angela, you are right! I live in North East Pa.and this area has the highest rate of tick born diseases in the country. People who haven’t been affected by ticks are in the minority.I got the shots years ago with no ill affects. Recently I was bitten and sent the tick away to be tested. It came back positive for Babesiosis, I had the bulls eye and yet I did NOT get sick….Yet our dogs have all had tick diseases, and my husband now has a pace maker from Lyme..He has had it 2x….We just do not understand this awful thing!
We need all the help we can get here! ?
I got the Lymerix vaccine back in ’99-’00 and didn’t have a solid bm for 3 years. Had to give up running due to knee pain.
This post is not anti-vaxx- it is anti-Lyme vaccine so please read WHY a vaccine won’t work for #Lyme. I wish it would! Try to give the benefit of the doubt here and read for yourself.
1st, there are 300 strains of Lyme and the vaccine only covers 1. Understand history of dangerous Lyme vaccine LYMERix that was pulled from market for injuring so many and know that the next gen will be similar. Many experts in the field agree the new Lyme vaccine (Valneva) will be equally dangerous and useless due to similar mechanism of action.
NOTE: LYMERix was pulled for injuring hundreds of patients–not for “low demand”, and not because of “anti-vaxxers.” It was hastily pulled after damning U.S. Food and Drug Administration hearings with vaccine experts and patient testimony (see below). Some are permanently disabled. The PR story was that it was pulled for “low demand.” That is false. See below data for the real story. Lyme vaccine will not cover all 300 strains of Lyme and it will not cover arguably worse infections (Bartonella, RMSF, Babesia, Powassan etc) transmitted by ticks and other vectors.
1) Pamela Weintraub, The bitter feud over LYMErix: Big pharma takes on the wrong little Osp 2001:
http://www.whale.to/m/lymerix8.html
2) Summary of 2002 meeting between Lyme Disease Association and FDA on LYMERix
Note in particular the comments of Donalds H Marks MD, PhD who was director of Lyme vaccine program for Aventis Pasteur, formerly Pasteur Merieux Connaught, the producer of the other Lyme vaccine (also OspA-based) that was never pushed to market. Despite phase 3 efficacy data (published in New Eng J Med in 1998, same issue as Steere et al’s report on LYMERix), the company quietly ended its Lyme vaccine program after LYMERix side effects came to light.
https://www.lymediseaseassociation.org/about-lyme/controversy/vaccine/261-lymerix-meeting
3) Marks DH Neurological complications of vaccination with outer surface protein A (OspA) Int J Risk Safety in Medicine 2011:
https://www.ncbi.nlm.nih.gov/pubmed/21673416
4) Latov N et al Neuropathy and cognitive impairment following vaccination with OspA protein of B burgdorferi J Periph Nervous System 2004:
https://www.ncbi.nlm.nih.gov/pubmed/15363064”