The Poisoning of Bangladesh: How Arsenic Is Ravaging a Nation
Now in his 60s, former shopkeeper Shahaz Uddin has been looking forward to becoming another white-bearded grandfather enjoying retirement. But there’s a signal that may be complicated — a warning sign in the spots freckled across his chest. The speckles of pigmentation start out black and then turn white, says Dr. Tariqul Islam, as he leans forward and examines Uddin. Like “raindrops on the sand,” he says, following the spatter across his patient’s skin. These are the telltale signs of arsenic poisoning.
Uddin lives in the village of Totar Bagh, an agricultural community of corrugated iron and concrete huts set amongst rice fields and woodlands to the east of Dhaka, Bangladesh’s capital. Colorful laundry hangs amidst palm trees over the earthen floor, as families go about their business of cleaning, cooking, and fetching water from shallow, hand-pumped wells.
It is the well water that has brought Dr. Islam to the village today. He is working with the University of Chicago and Columbia University to study the effects of long-term exposure to the famously risky element, arsenic. About half of the wells in their study area of 35,000 people in the region of Araihazar contain arsenic at more than 50 parts per billion, five times the World Health Organization standard of 10.
“I know this water is not good for my health, but there is nothing to do,” says Uddin. He tried installing another shallow well himself, but it was contaminated too. A deep well would have safe water, but at $1,000, it’s 10 times the cost of a shallow well and too expensive for villagers to dig without government or other outside support. He asked the local governing council for a new well, but they refused. “They told me to get better water.”
One villager who did get a new well is Piar Ali Shaheb, a building contractor who is also the local representative of the ruling party. When asked if his political connections helped, he smiles: “Yes, definitely.” As he is talking, a neighbor glistening with sweat just in from the fields approaches and begins shouting at him. He says he paid money to a local politician in order to get a safe well, but it had never been delivered. Many of the other villagers have the same story, and are also frustrated.
Shaheb, relaxed in his tank top and sarong, shrugs: “You gave the money to the wrong guy.”
Left with no alternative water source, Uddin, like most of his neighbors, is still drinking from his contaminated well. He spreads his hands before him and looks heavenward as his grandchildren play at his feet. “I have no alternative.”
Bangladesh’s contaminated well water is considered one of the largest public health crises in the world, and yet it remains relatively unknown outside of scientific circles. An estimated 40 million people — one quarter of the population — are exposed to drinking water contaminated with arsenic. While many people think of arsenic as the fast-acting homicidal agent beloved by the Borgias and their ilk, at the diluted levels found in drinking water, arsenic becomes a different kind of hazard: a tasteless, odorless, pernicious poison. Chronic exposure may lead to only a few visible symptoms (skin pigmentation on the chest, hands, and feet occurs in a minority of cases), but the poison is exceptional in its ability to silently attack multiple organs over the course of years, or even decades.
The result is that trace arsenic exposure in Bangladesh appears to have led to dramatic increases in cancers ranging from skin to liver to lung, in cardiovascular disease, and in developmental and cognitive problems for children. The Bulletin of the World Health Organization estimates that the invisible taint of arsenic in the country’s well water could now be responsible for as many as 43,000 deaths per year in the country.
A naturally-occurring metallic element, arsenic was first discovered in the country’s drinking water more than two decades ago. At that point, dismay led to widespread water testing, but relatively little has been done to directly address the problem in recent years. Yet researchers say there is no question that the mass arsenic contamination is solvable in most cases by drilling wells deeper than 500 feet. Some deep wells could provide for several hundred villagers, while the shallow wells they would replace usually serve only one household. Geologists say that enough wells and other types of safe water projects to supply water to the worst exposed 20 million people could be provided relatively quickly — and that such improvements could gradually be expanded to other at-risk populations.
“If they are properly sited in areas of greatest need, even a small increase in the rate of installing deep tube wells could bring arsenic poisoning to a virtual end in five to 10 years,” says Peter Ravenscroft, a groundwater expert who has worked on the arsenic issue for more than two decades and is currently advising WHO and UNICEF on new arsenic mitigation guidelines.
And this raises a troubling question. If the problem is solvable, if ending what WHO once dramatically called “the largest mass poisoning of a population in history” involves a straightforward fix, why hasn’t that simply been done?
To appreciate why that question is such a complicated one, one has to go back to the moment in time several decades ago when public agencies decided to first tackle water quality problems in Bangladesh.

In the 1970s, hundreds of thousands of people a year in Bangladesh were dying from cholera and other diarrheal diseases. UNICEF and other international organizations were on a mission to help countries access clean water throughout the developing world. In an effort to get people to stop drinking dirty surface water, they worked with the Bangladeshi government to promote the use of shallow, hand-pumped wells.
It seemed to be a textbook solution: cheap; easy to maintain; a collaboration of government, community, and private sector; and focused on attacking the root cause instead of the symptoms. An estimated 10 million hand-pumped tube wells were drilled across the country, at first by the government, UNICEF, and other donors and NGOs, and later by individuals and families. The project appeared to be a roaring success. The purity of the water was even tested by the British Geological Survey. Unfortunately, they did not test for arsenic.
The arsenic in Bangladesh’s shallow aquifers is naturally occurring, the result of a confluence of interlinking factors. Particles of iron oxide with arsenic chemically bound to them are carried into Bangladesh from the Himalayan Mountains by the fast-moving Ganges and Brahmaputra rivers. These particles are carried from the cold, high altitudes to the sluggish waters of tropical marshes and swamps, where they are broken down by oxygen-seeking bacteria, releasing the arsenic into the groundwater. This is the layer of water tapped by high-density hand-pumped tube-wells used by the rural population. Agricultural laborers are particularly susceptible to the poison, as they work long hours in the hot sun, drink a lot of water, and rely on rice (which also takes up arsenic) as their staple food. Already weakened immune systems from poor nutrition and a paucity of health care will compound the effects.
After the arsenic was discovered, the World Bank led an effort to test more than half the country’s wells. A wide swath of the wells was found to be contaminated, thought to expose more than 57 million people. Educational programs urged people to seek out new sources of drinking water and contaminated wells were marked with red paint. But little was done — aside from the digging of a limited number of new wells — to tap cleaner supplies. Many of those who could switched to safer wells, but most people had no options.
Millions were left drinking the contaminated water.
As the case of Uddin and his neighbors illustrates, local patronage and nepotism are part of the failure to deal with the problem. But that’s only a symptom of the larger and more daunting obstacle, policy experts say: a lack of political will.
“There is a corporate psychology aspect to this public health issue,” says Ravenscroft, who has advised both UNICEF and WHO on the issue. The scale of problem has been an obstacle to sustained action by donors, he explained: “I think they are afraid of taking responsibility for a problem they think is too big for them.”
As with so many things in public policy, it’s not the technology that’s the barrier to change: it’s the implementation. At this point, the consensus among engineers and geologists is that deeper wells, lower than 500 feet, would provide arsenic-safe water that could each serve 10 or more families. Filtering surface water can also work in some cases. The better and longer term — but more expensive — solution is providing piped water to an entire community using a central filtration plant, which has so far been tried successfully in a handful of test cases.
At issue is a question that goes beyond the case of Bangladesh to a larger dilemma facing the powerful institutions that get involved around the world: Who is responsible when an effort to do good ends up doing harm? The charity or foreign aid agency? The government that received the aid? The consulting firms that worked on the project? With no accountability in sight, the people who were supposed to be the ones being helped are left to pick up the pieces.
In the wake of the massive testing program after the arsenic was discovered, interest from government and donors faded in the last decade. Dr. Kazi Matin Ahmed, Chairman of the Department of Geology at the University of Dhaka who has been working with the Columbia University team, says that the Bangladeshi government possesses most of the resources to address the problem.
And he’s frustrated that that hasn’t happened. Surveys by the Bangladeshi national government show that arsenic contamination in the drinking water barely changed between 2009 and 2013 — the most recent data available — suggesting that millions of people continue to be poisoned every day: “Certainly I am not happy because in the last 20 years, no one should have drank this water,” Ahmed says.


In the district of Faridpur, a rural area near Dhaka on the banks of the Padma River, Abdul Latif Sheikh lives in what seems like an idyllic village compound, with a brown calf in the yard and the sound of roosters crowing as they bobble around the water pump. Sheikh is strapping and tall, but his voice rings with disappointment.
He and his wife Rokeya drank for years from arsenic contaminated well. Rokeya has dark marks on her hands, wrists, and feet. She picks at them as he talks. She is sick and losing weight. She has no time to go to the doctor; since her husband cannot work, she must bring in the money. Their son and daughter live with them.
“If we die, who will look after our family?” she asks. Since she knows her well is contaminated, Rokeya fetches water from the well at the local fisheries office. Many in the village do the same, assuming that because it is a government well, it is safe. In fact, the well has no markings indicating it has been tested. A subsequent test by the Columbia team, done at this reporter’s request, revealed that it had arsenic levels 10 times the safe limit set by WHO.
“You cannot prevent arsenic at the individual level, you really need community based measures. You need nationwide, global interventions,” says Ana Navas-Acien, an epidemiologist specializing in preventive medicine at Columbia University. “We cannot do practically anything at the individual level.”
Last year, the Bangladeshi rural public works department proposed a $250 million plan to address the arsenic crisis. But it has yet to be approved by the government leadership, and some experts, including public officials, are skeptical it will actually happen, noting that politicians’ promises to address the arsenic problem have fallen through many times before. Bangladesh is already well-known in public health circles for its successful programs to end open-defecation and reduce child mortality. Arsenic poisoning is perhaps more confounding because the effects take years to occur.
“Policymakers don’t get alarmed by silent killers,” says Habibul Ahsan, a professor of public health and associate director of the Cancer Research Center at the University of Chicago, one of the chief health researchers in Araihazar. A study he worked on with Columbia University known as HEALS found that for people drinking the arsenic tainted water, the exposure could account for one in five deaths.
The Bangladeshi government has installed more than 200,000 new tube wells in the last decade, but they are part of general infrastructure development and not intended to address the public health problems related to arsenic contamination. A report by Human Rights Watch found that the wells often appeared to be going to politically connected villagers, echoing a similar finding by Alexander Van Geen of Columbia.
Publicly, the government denies the allegation of corruption or nepotism. “We are working fully and wholly and religiously for arsenic,” says Abdul Malek, the Secretary of the Local Government Division of the Bangladeshi government. He adds that the Human Rights Watch report is “false, truly false, highly fabricated, and highly political biased.”
Privately, however, a senior government official acknowledges that local politics often dictate who gets wells.
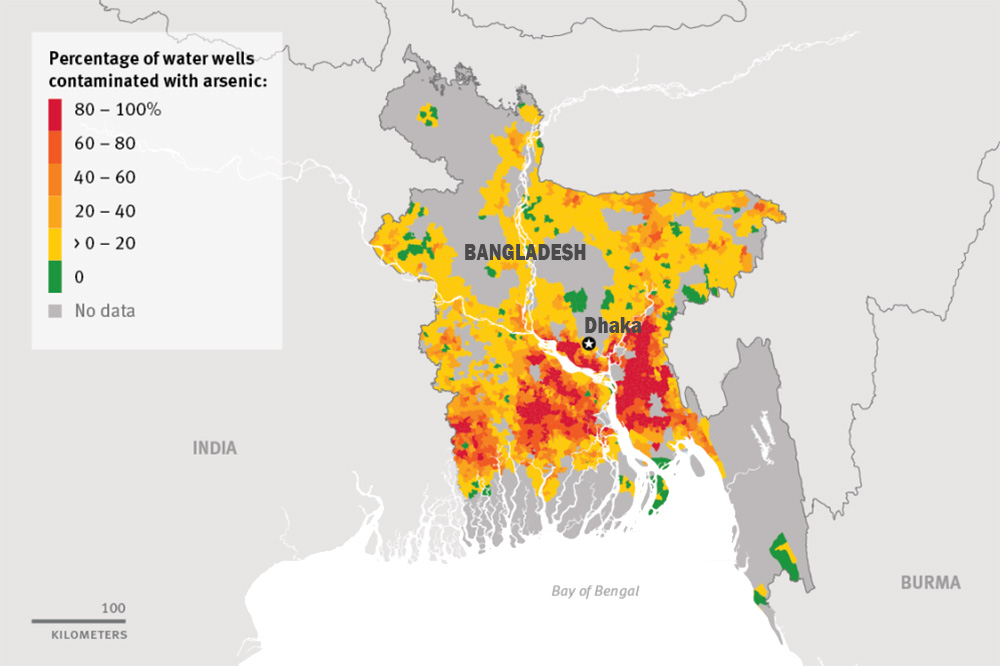
Arsenic is not just a Bangladesh problem — it can be found in drinking water supplies around the world. Maine, Massachusetts, Texas, and half a dozen other states have all had arsenic contamination problems, says Joseph Graziano, a professor of environmental health sciences and pharmacology at Columbia University. Population-level contamination, on a smaller scale than Bangladesh, occurred in Chile and Taiwan decades ago and the long-term effects of the toxic substance are still being studied. In Chile, the entire city of Antofagasta was poisoned. “We have more than 40 years after exposure ended and we still see people with excess risk of developing cancer today,” says Dr. Catterina Ferreccio, the deputy director of the Advanced Center for Chronic Diseases at the University of Chile. She describes entering a hospital ward back in the early 1970s and seeing rows of children who had had heart attacks from being exposed to arsenic.
Meanwhile, the Bangladeshi government has largely downplayed the problem. The government has still not adjusted its arsenic safety level to meet the decades-old WHO standard. This means that officially, “only” about 20 million people are considered exposed to arsenic; WHO estimates the number is closer to 40 million. Further, the Ministry of Health official in charge of monitoring arsenic says the number of people actually affected is far less: that just the 65,000 people displaying visible skin lesions have actually been poisoned.
“Arsenic is not now [a] problem [in] Bangladesh,” says Dr. Faruk Ahmed Bhuiyan, a senior official at the Directorate General of Health Services in charge of overseeing the arsenic issue. His colleagues add that his program did not see any connection between cancer or cardiovascular issues and arsenic poisoning. His office estimates that only 100 or 200 people die each year as a result of arsenic poisoning. He and his colleagues say they were unaware of either the WHO Bulletin study or the Columbia/Chicago HEALS study, or any of the epidemiology linking arsenic with chronic diseases.
In fact, skin lesions are a poor proxy for arsenic poisoning because they only occur in a small minority of cases, says Graziano. Graziano is a co-author of the HEALS study, which closely tracked the dose-response effect in a population over time, making it the most definitive study of arsenic poisoning so far. In most cases, the effects of arsenic poisoning may remain hidden for years until the damage is already done, he says.
Meanwhile, donors and international agencies have largely turned away from dealing with the problem. UNICEF, the World Bank, and WHO do not have any major projects focused on arsenic mitigation, nor do bilateral donors from the United States or Europe. “It’s gone totally off the donor radar,” says Peter Kim Streatfield, an emeritus scientist with the International Center for Diarrheal Disease Research, Bangladesh, one of the country’s premier public health research institutions.
The politics of aid — and many competing priorities — make large-scale action from one institution difficult, even for the agency that was so intimately tied to the origin of the problem, says Shima Islam, a spokesperson for UNICEF. “Raising $400 million for just water in one country would be an extremely difficult task,” Islam says. “If we just concentrated on water in one country, the donors themselves would be asking, ‘Well hang on a minute. You’ve forgotten about health, you’ve forgotten about education, you’ve forgotten about child protection.’ There are so many other issues in this country and we have to prioritize.”

Several years ago, though, UNICEF conducted clean-up demonstration projects across a handful of the worst affected villages. Water experts worked with local leaders to put in community-wide water systems that have virtually eliminated the problem — for now.
In the village of Batachow in Comilla, Southeast of Dhaka, the agency worked with the village to install a piped water facility using a central filtration plant, consisting of brewery-sized gleaming tanks and trellised water filters. As a result, Batachow, which was once almost completely contaminated, now has safe water.
“It was beyond our imagination that we would have a water supply solution like this,” says Mamunur Rashid, a member of the village water committee. The whole village receives water for two hours in the morning and two hours in the evening, and it also goes to a school and community clinic.
So far, this “arsenic safe village approach” has only been done in a small number of communities to demonstrate to donors and the government what a possible solution would look like. UNICEF provided the initial funding for set up — about $50,000 — and now it is up to the village to pay for maintenance with fees.
Shafiqur Rahman, the plant’s caretaker, suffers from residual arsenic poisoning. He explains the workings of the plant, showing how water comes up and runs through various filters for arsenic, iron, and manganese. Pointing to a box with flashing lights, he says it contains “medicine,” actually sodium hypochlorite. So far, he adds, the machinery has worked well: “Insha’Allah it will last long.”
But as much as people in the village embrace their new water system, raising enough funding for maintenance remains a struggle for the community. And neither the government nor the public health organizations have plans to invest further at this point.
“If it’s not well maintained, then it all goes to waste,” says Nargis Akter, a UNICEF water expert.
Sam Loewenberg is a journalist who covers the intersection of global health, business, government and politics. His articles and photography have appeared in The Economist, The New York Times, The Guardian, Time, Newsweek, Forbes, Portfolio, The Atlantic Online, Fortune, The Nation, The Washington Post, Slate, Salon, and The Lancet.
This report was funded in part by the European Journalism Center via its Innovation in Development Reporting Grant Program (www.journalismgrants.org)











Comments are automatically closed one year after article publication. Archived comments are below.
Saitrth Bldg Plot 82
304
I have been studying heavy metallic contamination of water in India and my findings are almost similar to what has been mentioned by the author. There is a solution but it is not implemented because of lack of political well.
thanks for valuable report on ARSENIC.