In Hot Pursuit of a Single Shot to Defeat the Flu
Flu season may prove to be worse than usual this fall and winter, some early reports suggest. So it’s wise to get your annual shot.
But while researchers try to tailor each year’s vaccines to protect against anticipated strains of influenza, the virus sometimes outwits them — mutating faster than manufacturers can produce a closely matching vaccine. What’s needed, experts have been saying for more than a decade, is a universal vaccine: one that would work against all strains of influenza and last for years.
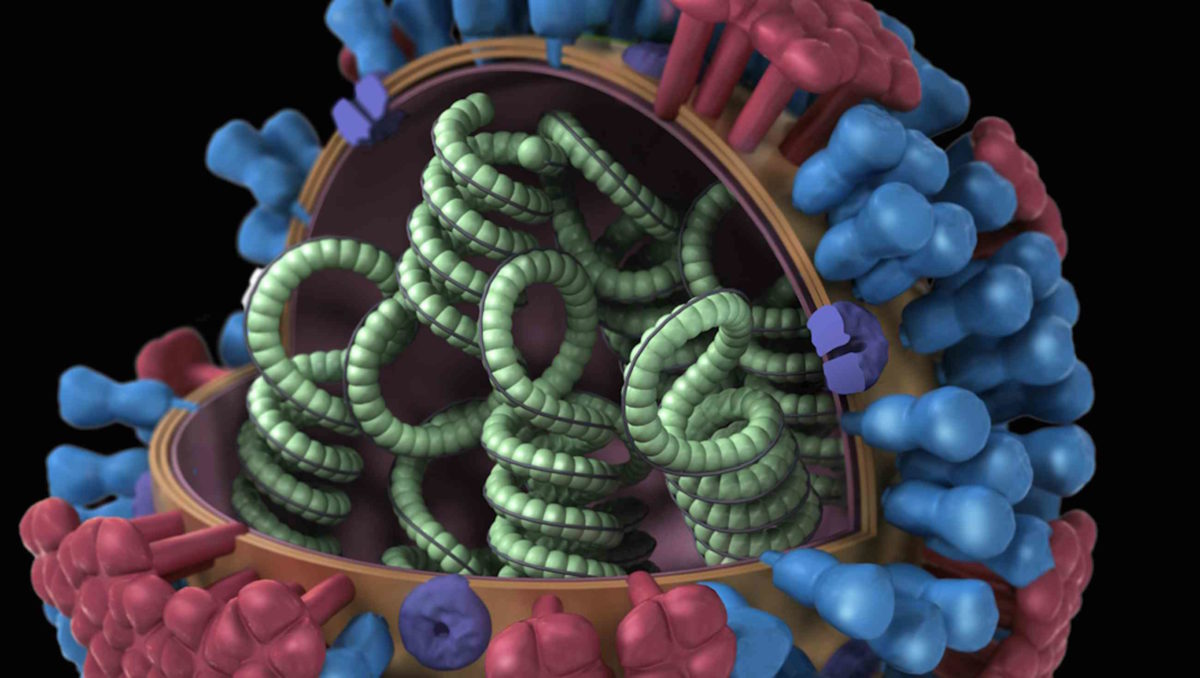
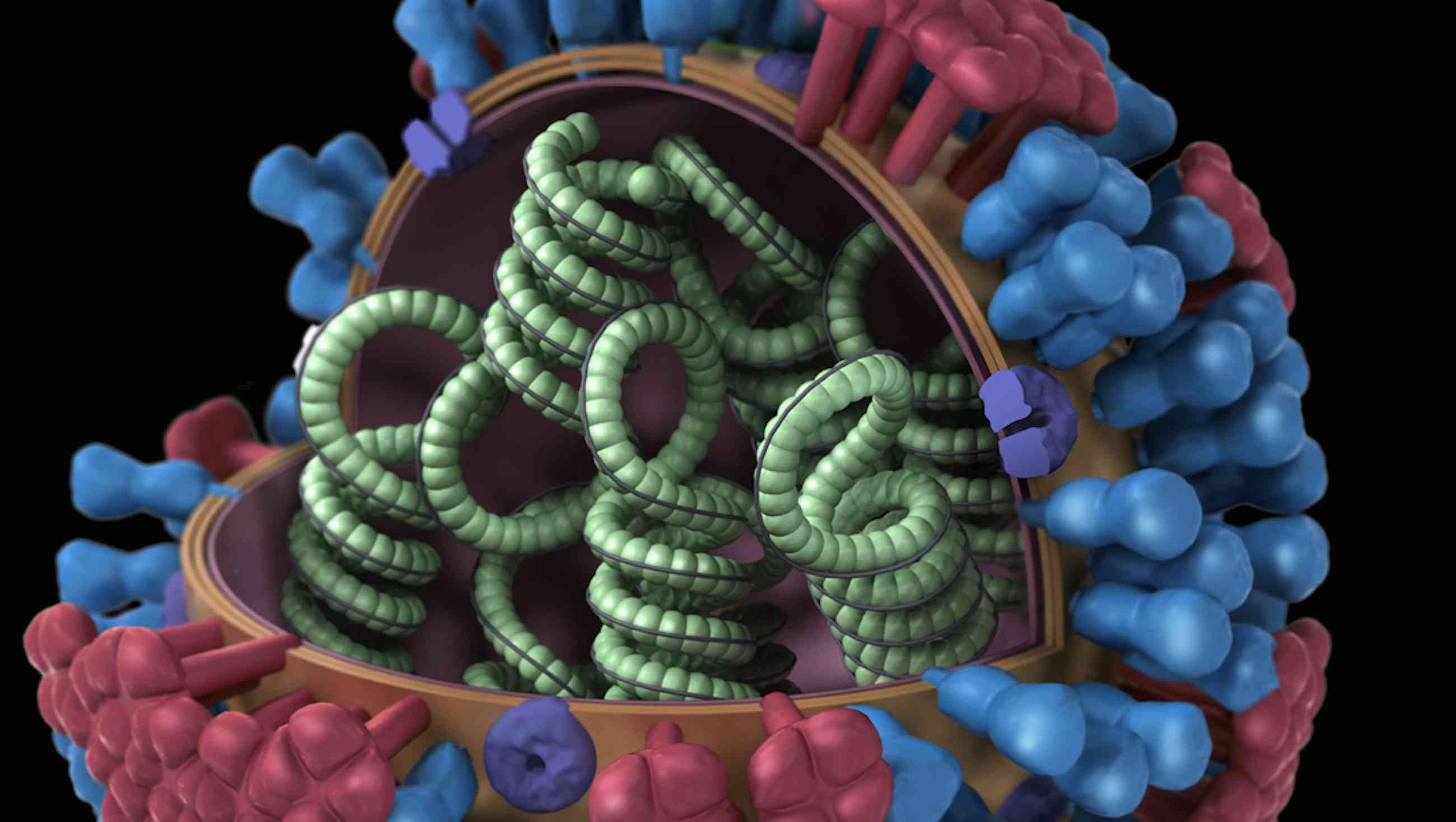
The structure of an influenza virus. Nearly 100 years after the Spanish flu pandemic, the world remains vulnerable.
Visual: Centers for Disease Control and Prevention
Such a vaccine would protect not only against the seasonal flu, which kills tens of thousands of Americans annually, but also from pandemics like the Spanish flu of 1918, which killed as many as 100 million people worldwide. (That is the equivalent of 400 million people today — nearly 50 times the population of New York City.) Pandemic outbreaks occur when populations are exposed to a new strain for the first time and thus have little or no immunity.
At a gathering of flu researchers on Monday at the Smithsonian National Museum of Natural History in Washington, the flu policy specialist John M. Barry said the need for such a vaccine was obvious. “We need to put a lot more resources into vaccine research, particularly universal vaccine,” said Barry, author of “The Great Influenza: The Story of the Deadliest Pandemic in History.” And meanwhile, he added, manufacturers need better technologies to make seasonal vaccines.
Anthony Fauci, director of the National Institute for Allergy and Infectious Diseases (NIAID) for the past 33 years (under six presidents), has long agreed on the need for a universal vaccine, a point he reiterated during the Monday event as well as in a research paper and an opinion essay, both published this fall. In a perfect world, this one-time flu shot would last a lifetime and protect against all strains of the virus.
Today, the world remains vulnerable to a pandemic flu nearly 100 years after the Spanish flu, Fauci said, adding, “Our public health structure has improved greatly, but without a universal vaccine, a single virus would result in a world catastrophe.”
But he’s optimistic that such a vaccine is within reach. “I think from a scientific standpoint we will get there,” he said.
Several teams, including some at NIAID, have made progress in developing vaccines that provoke antibodies differently from standard vaccines, and thus potentially across more strains, Science News reported last month. But it remains unclear whether this approach will protect humans from many strains.
Until flu vaccines improve, public health officials must confront outbreaks rationally and tell the truth, Barry said. In 1918, he went on, some national public health leaders issued false reassurances, saying that standard flu precautions would be sufficient. Communities that responded accordingly fell apart, in part because no one would share food, touch anyone, or make deliveries. San Francisco was a notable exception; it maintained some social order by issuing extra warnings and enlisting volunteers to deliver food and medicine.
During the 2009 H1N1 flu pandemic, which killed 12,469 people in the U.S. and up to 575,000 worldwide, the leaders of some nations went overboard in their efforts to screen travelers or quarantine suspected carriers of the virus.
“Which means I think maybe the biggest challenge in the public health community is to get political leaders to make rational decisions in crisis situations,” Barry said. “And that is where the leadership in the public health community really matters.”