In the years since a family member of mine started taking methadone, a drug that helps him avoid the excruciating withdrawal symptoms and intense cravings that come with an opioid use disorder, he’s attended the funerals of three of his closest friends with whom he used to use drugs. The number of acquaintances he’s lost is in the double digits.
Methadone might have saved them — if only they could have picked it up from their local pharmacy.
Like heroin or oxycodone, methadone stimulates the opioid receptors in the brain. The difference is that while heroin rapidly floods these receptors leading to an intense high, the effect of methadone is more gradual and long-lasting. At the appropriate dose, my family member (whom I’m not naming due to the continued stigma surrounding opioids) and other patients can get full days of relief from pain, withdrawal, and cravings, without the intoxication. But methadone is tightly regulated. Rather than pick it up from the local pharmacy, patients have to visit a specialized clinic — often daily — to get each individual dose.
In March 2020, concerns about Covid-19 led the Substance Abuse and Mental Health Services Administration, or SAMHSA, to relax those restrictions. The agency announced that states could request an exception allowing clinics to offer a greater amount of take-home doses— up to 28 days — for patients the clinical team believed were stable and could safely handle the medication. Some clinics embraced the opportunity. In a multistate survey of 170 opioid treatment programs, about half followed the relaxed SAMHSA guidelines for newly enrolled or less stable patients. And two-thirds of the clinics surveyed offered their stable patients a full four weeks of take-home doses.
The pandemic provided the natural experiment to demonstrate that loosening regulations on methadone in the U.S. was safe for both patients and communities. More than two years later, on July 13, researchers at the National Institute on Drug Abuse and the National Center for Injury Prevention and Control published some of the most powerful results of that experiment. While deadly overdoses involving opioids rose to staggering heights in the U.S. during the first year of the pandemic, the percentage of overdose deaths involving methadone decreased.
Some were concerned that allowing patients more take-home doses would raise the likelihood they would take multiple doses at once and overdose, but new research found that wasn’t the case. In fact, another 2022 study shows that when two clinics in Oregon offered additional take-home doses for patients who’d been in treatment for 180 days or more, treatment success actually improved. More people continued treatment and fewer relapsed. The patients said the increased take-home doses made them feel trusted and provided them with more time to dedicate to their careers and families.
In November 2021, SAMHSA announced that it would extend the loosened regulations for another year. Meanwhile, lawmakers have introduced a bill that would reform methadone care. But many clinics chose not to expand take-home doses despite the option to do so. Loosening state regulations on existing methadone clinics isn’t enough. If SAMHSA and the federal government hope to save lives, they should release methadone from the siloed clinics that make using it incredibly burdensome to patients.
We already know methadone works. Allowing people to pick up a week’s or month’s supply at their local pharmacies will make it work better and for more people. And methadone not only helps people maintain sobriety — it saves lives. A February 2020 study, for instance, compared patients who were prescribed methadone or buprenorphine, a similar, but less potent, medication used to treat opioid use disorder, with patients who had undergone other treatment pathways, such as residential treatment and behavioral therapies. Only treatment with either medication was associated with a reduced risk of overdose —76 percent within 3 months and 59 percent within a year. A 2015 study from England found similar results: Patients who received psychological therapy alone were twice as likely to die from an overdose than those who received methadone or buprenorphine.
In part because buprenorphine may have a lower risk of overdose than methadone, it has fewer restrictions. The drug has long been a controlled substance, but, unlike methadone, patients can obtain buprenorphine from a pharmacy and take it at home. While buprenorphine is as effective as methadone at higher doses, studies show that when patients were given the lower doses of buprenorphine most commonly prescribed, they were much less likely to continue treatment than patients who were treated with methadone. That was the case for my family member. Before methadone, he tried buprenorphine, in part because it was easier to access, but he never felt stable on it. “I always felt like I was about to fall off a cliff,” he said. One day he’d seem perfectly fine. The next day he’d slur his speech a little. Another day, I’d get a call that he needed to be bailed out of jail.
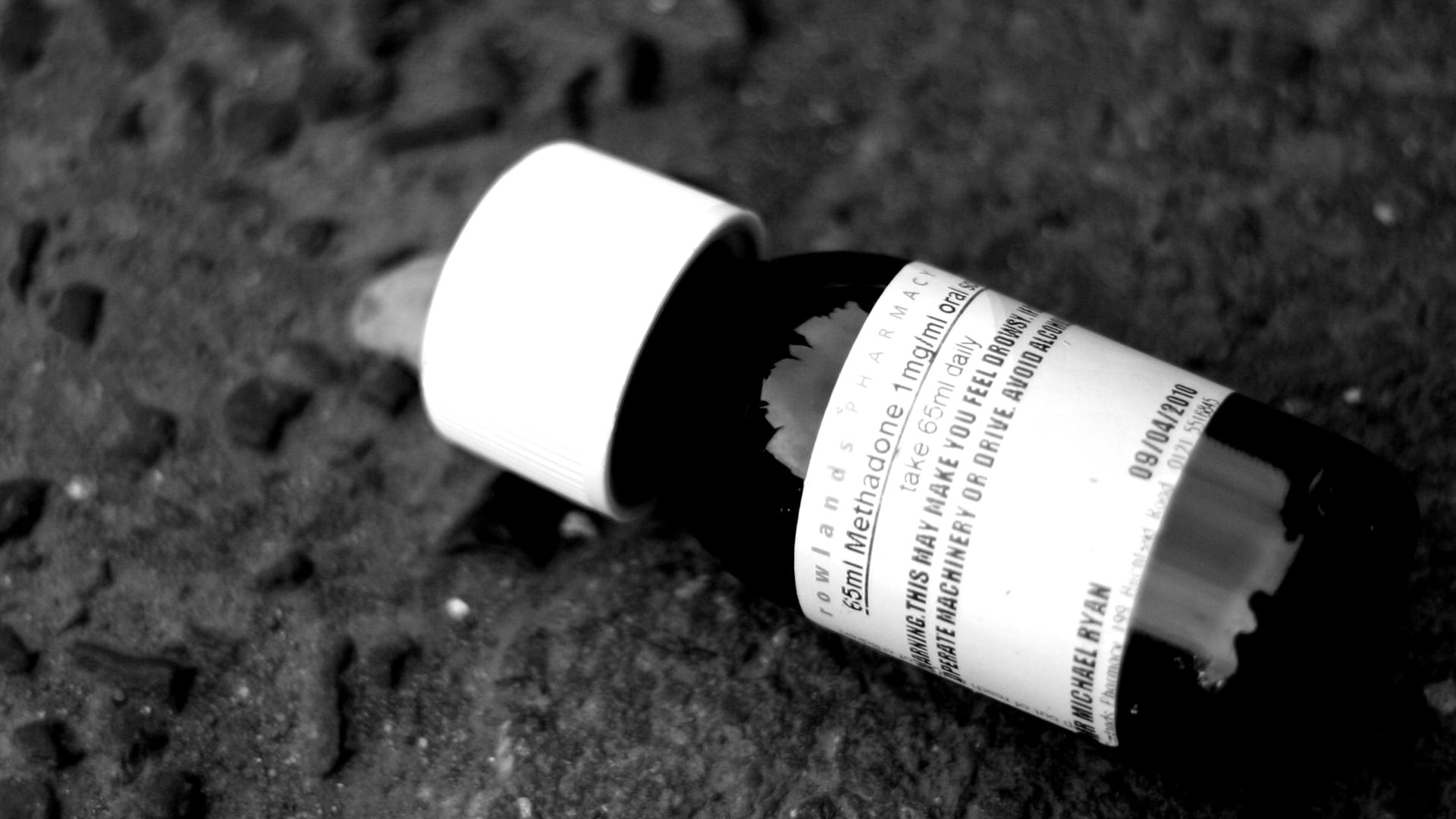
That’s why he chose methadone, despite the layers of regulations enacted in the 1970s that meant that rather than picking up a monthly supply at his local pharmacy, he’d need to go to the opioid treatment center day after day, so a nurse can watch him place the liquid into his mouth and swallow.
Eventually, after proving their reliability to their counselor, a patient may earn individual doses to take home. That same counselor also has the authority to withhold that patient’s dose for any reason, from a positive drug test to subjectively inappropriate behavior at the clinic to possession of an out-of-date bottle cap. This makes treatment inconsistent and unpredictable.
In a small qualitative survey published in 2021 in Harm Reduction Journal, patients repeatedly said that daily clinic visits interfered with their ability to maintain steady employment. It’s not just picking up medicine. Patients often attend mandatory counseling sessions and produce urine samples on-site (with supervision) to prove they’re taking the medicine and haven’t relapsed. Some of these services are inconvenient. Some are humiliating. Most also drive up the cost of care (and profits at the many for-profit facilities). At any time, my family member pointed out, a patient with take-home methadone doses can be called in for a bottle recall, in which case they have a few hours to retrieve any used and unused take home doses and bring them to the clinic before it closes.
Health researchers and policy analysts have long lamented these regulations, and often called for them to be overhauled. Other countries, such as Canada, Australia, and the United Kingdom, have allowed methadone to be picked up from regular pharmacies since the 1960s and ’70s. But stigma, racism, and the distrust of patients have prevented the U.S. from doing the same.
While the July data shows that patients were just as safe, if not safer, when offered more take-home doses during the pandemic, the North Carolina survey suggested the community remained safe as well. Only six out of 87 patients surveyed sold or shared their doses in the summer of 2020, often with the stated goal of helping a friend who needed methadone.
There are a lot of ways the U.S. can improve its treatment of people who use drugs, such as opening safe consumption sites, distributing the overdose-reversing drug naloxone, and making it easier for doctors to prescribe buprenorphine. But one of the simplest and most effective is right in front of us: pry methadone from the clinics that shackle those who need it. The U.S. is currently considering ways to reform opioid treatment centers, but with overdoses growing more frequent and more deadly, now is the time to recognize that one of the best tools to prevent overdoses has been here all along, if only we could forget the opioid treatment centers and pick it up from the pharmacy.
Emma Yasinski is a science journalist whose work has appeared in The New York Times, National Geographic, The Atlantic, and other publications.
If you or someone you know needs help with a substance use disorder, you can reach the Substance Abuse and Mental Health Services Administration’s National Helpline at 1-800-662-HELP or the National Drug Helpline at 1-844-289-0879. You can also visit findtreatment.gov.










Comments are automatically closed one year after article publication. Archived comments are below.
I was taking 120 mgs of methadone per day. I had lost my medical insurance and the ability to continue at a pain clinic. After a few years or so I stopped… cold turkey. I no longer had the pain that justified taking it. I was awake for about six weeks. Just mild chills and the restless legs when trying to lay down and sleep. Some people take quite a bit more and I’m sure their withdrawals can be absolutely horrible. I wish I had known about Kratom at the time! I have never used Kratom to relieve withdrawals from methadone or anything else, but it might be worth a try for someone who needs that. It is an opiate antagonist, and it is legal. Use the “Red Vein” variety. You should be able to get a kilo for about $80 or less online. Just a few spoonful’s in some orange juice or apple sauce. I half fill a 12 oz., plastic, orange juice bottle, drop in a few teaspoons and shake. You cannot eat too much of that powder on a regular basis because all that fiber will block you up and that could be a serious problem requiring an embarrassing ER visit. The FDA, probably fueled by Big Pharma, made some false claims about kratom and tried to make it illegal but it did not work thanks to the American Kratom Association and some senators/congressmen.
I don’t agree about that when I did methadone it doesn’t block the optiod blockers methadone made me do more drugs. But 5 months ago I got on suboxone and I can say it works great I don’t even think about drugs anymore and now I’m normal to have a job and be a part of society again
Methadone is a great harm reduction tool. I’ve seen people do great things while on methadone maintenance.
I have also seen how hard it is for people to taper off of methadone.
There are so many harm reduction tools available to us right now, and most of them are hard to access. We need to make suboxone and methadone easier to get for people struggling with opioid use disorder.
I have been clean for seven years with the help of kratom. It is a leaf from southeast Asia. I take it three times a day Nd don’t think about it when I don’t have it. I coupled my kratom use with an active change in my attitudes and ideas. NONE of these harm reduction tools will work without instituting some sort of recovery program. Self awareness and getting to the root of the disease is very imlortant.
Methadone saved my life. I have never met more caring people than the clinic I go to. Most people don’t get take homes because they blow their UAs with weed or other drugs. I had botched surgeries, severe nerve pain and wanted to blow my brains out. Ended up in pysch facility. So they took away all my meds. My pain doc previously wouldnt give me back fentanyl patches because she was afraid of her lisc. and all the stuff going on. I havent been to the ER in 4 years !!! Best nerve pain reliever. Which is a miracle. I function everyday and havent had the pain I did in a long time. If your drooling in your chair or not functioning maybe your dose is too high. I’m so tired of drug addicts complaining about methadone. Medicaid pays for cab rides and all treatment at my clinic. You get treated better than pain patients who you caused to lose their meds, jobs, lives and you bitch because you gotta carry a box. Dont go to the clinic if it sucks so much. No one owes you anything.
I know first hand, if people could get methadone at a local pharmacy, it will save life’s, because alot of people where l live in KENTUCKY, DONT HAVE TRANSPORTATION TO A OUT OF COUNTY CLINIC TO GET THEIR DAILY AND FOR THOSE WHO CAN , ITS A BLESSING, I ALSO KNOW PAITENTS WHO HAVE BEEN GOING OVER 2 YEARS AND STILL ONLY GET WEEKLY TAKE HOMES, ITS VERY STRESSFUL NOT KNOWING HOW YOUR GOING TO GET THEIR EVEN WEEKLY, AND THEY SHOULD LET YOU GO TO A PHARMACY FOR DRUG TEST TO OR LOCAL HOSPITAL , THIS IS 2022 NOT 1970S, HOPEFULLY THEY WILL CHANGE SOON,
I’m sorry but if you want to get off options for good and not keep on going to the methadone clinic then I’d have to disagree with you because a week kicking heroine compared to 6to a year kicking methadone and that’s tapering down (I’ve done it like 6 different ways and methadone is not the way to go ) unless you plan on going forever
But you are tied to a Methodone Clinic 5 days a week? Newer drugs hit receptors without dangerous withdrawals . Since Methodone is a long duration med, if you stop using it a fews days may be ok .but long term withdrawal from Methadone is more painful that other withdrawals Just my opinion drug counselor & harm reductionist
Do you believe kratom has a place in the community as a harm reduction tool?
Why is this not being investigated?
Billions in Healthcare Fraud by trusted cancer doctors putting cash before patients. That’s right, trusted cancer doctors killing vulnerable patients for money. This “hub and spoke conspiracy” to defraud government healthcare programs ( Medicare, Medicaid and TriCare ) was perpetrated by Amgen and J&J. as well as their co-conspirators (cancer doctors – see attachment) :
https://www.washingtonpost.com/business/economy/anemia-drug-made-billions-but-at-what-cost/2012/07/19/gJQAX5yqwW_story.html?utm_term=.69225f3f7117
While killing innocent patients Amgen, J&J and their co-conspirators also defrauded investors and made illegal tax deductions for the bribes. It’s pretty simple “Amgen/J&J can’t deduct illegal kickbacks and doctors can’t accept bribes!”
So until big drug/biotech stops paying billions In kickbacks to greedy doctors our healthcare systems will be destroyed. Of the $3 trillion per year in US healthcare expenditures, $1 trillion is fraud. So it doesn’t matter whether it is kickbacks to doctors for opioids or biotech the real addiction is greed! The kickbacks are illegal and someone needs to go to jail!
So why is this not being investigated
I tried the methadone route. God forbid if something happens and you can’t get your dose and end up in withdrawal! Death is the most wished for state for at least the 1st month. Withdrawing from opiates is easy comparatively speaking. And, depending on what state you’re in, your dose is decided by lawmakers, insurance companies, etc. Prepare yourself for an everyday regimen for months before you ” earn ” the right to get your medication for 2 straight days and don’t forget to bring your lockbox! And standing in long lines and planning your life around the hours these clinics are open. Frequent drug testing and mandatory counseling are often required. Thanks for the help!!!
I was on methadone for 8 years it’s artificial heroin I sat in a chair slept and drooled lost 8 years of my life I have CRPS the most painful condition known to man methadone is crap and I’m tired of not being able to get the meds I need because of drug addicts
Try kratom. It is a godsend for people with complex regional pain.
Thats just legal herion that is controlled by the government
The opioid crisis I face is the complete inability to get proper pain management now that I got through most of my life never abusing any substance, but now am in complete chronic pain. I’ve been through the gambit of chemical roulette trying the options other than opioids and suffer now from a myriad of side effects from the biologics to nsaids. I just want the pain to subside but keep getting treated like a druggie when I ask for opioids. I’m about at the end of my rope..
23 years I have been to and from my MMT clinic. I stated like everyone else “mostly” every day trip. Did my counselor meetings. My UAs drug test.
Every 3 months 1take home in a lock box that anyone that were familiar would look know thats Methodone. Some of the other patients have had there meds box snatched from them in daylight. Now the have no medicine no way of proveing this happened. So they become sick. Then it’s buy more Methodone on the street which coast even more than the 13 or 17 dallors they just paid per day. Now it’s at least a Dallor a mg . Most people are at 50 an up so if they don’t want to be sick to work or just live a pain free day . It’s 50 dallors a day now . So 13 for 92 a week to 50 mg for 7 now 350. At 1$ mg.
All for doing what was asked of them so that they could have a reflection of normal life. Give us a chance to have what you would want you or your family if this was not for the absolute grace of for their go I….
What a bunch of bullshit. I was on methadone for almost 5 years and it sucked the life out of me. I was still getting high everyday even tho I was on it. Just another ball and chain
Methadone is just another high and another addiction
Methadone ruined my life when I needed change! This medicine is another way for the government to make money off of our disease!
Yeah, just get them addicted to something much worse, that’s the answer. I was an opioid addict for 12 years went to methadone for @ 2years. When I tried to get off the methadone I almost died and ended up in the hospital. Methadone is not the answer. But I have been clean for 8 years now.
Might be the most ignorant article I’ve read on methadone. Trying to help declining sales? Ever hear of kratom?
Heard its desdly also
My sentiments exactly. A lot of these recovery specialists say they believe in harm reduction but when you ask them about kratom they turn their noses up at it. We have the most accessible And safe alternative right in front of us and no one can see it! Seven year kratom consumer here and my whole life has been turned right-side up! I wouldn’t be here without it!
Unfortunate that insurance companies tout the 6 month heroin blocker implant as too expensive yet the destruction addiction costs society costs us billions of dollars.
As a former methadone patient who switched to suboxone when my clinic ‘recalled’ me, I’m glad to see we may finally be moving away from clinics. In my experience, clinics OFTEN bully patients and drag out treatment because of financial issues. Seeing methadone go to pharmacies would probably benefit a LOT of addicts already in recovery and those who aren’t ready yet. Going to a clinic 6 or 7 days a week for at least 2/3 months to receive just one additional take home has always been ridiculous in my opinion. And the price structure at far too many clinics isn’t ideal, and often is prohibitive. I know it was for me!
You know what I know . This I’m on this side of the window or desktop. That power and shameful let me make this just as painful as I can. “Tell them your sin so they can sharpen the knife” kinda relationship. It would be awesome if all that’s promise would come to pass.
Do you seriously expect anyone to be able to read this chopped up, trainwreck of a post? How about “you” try to read this before you post it.