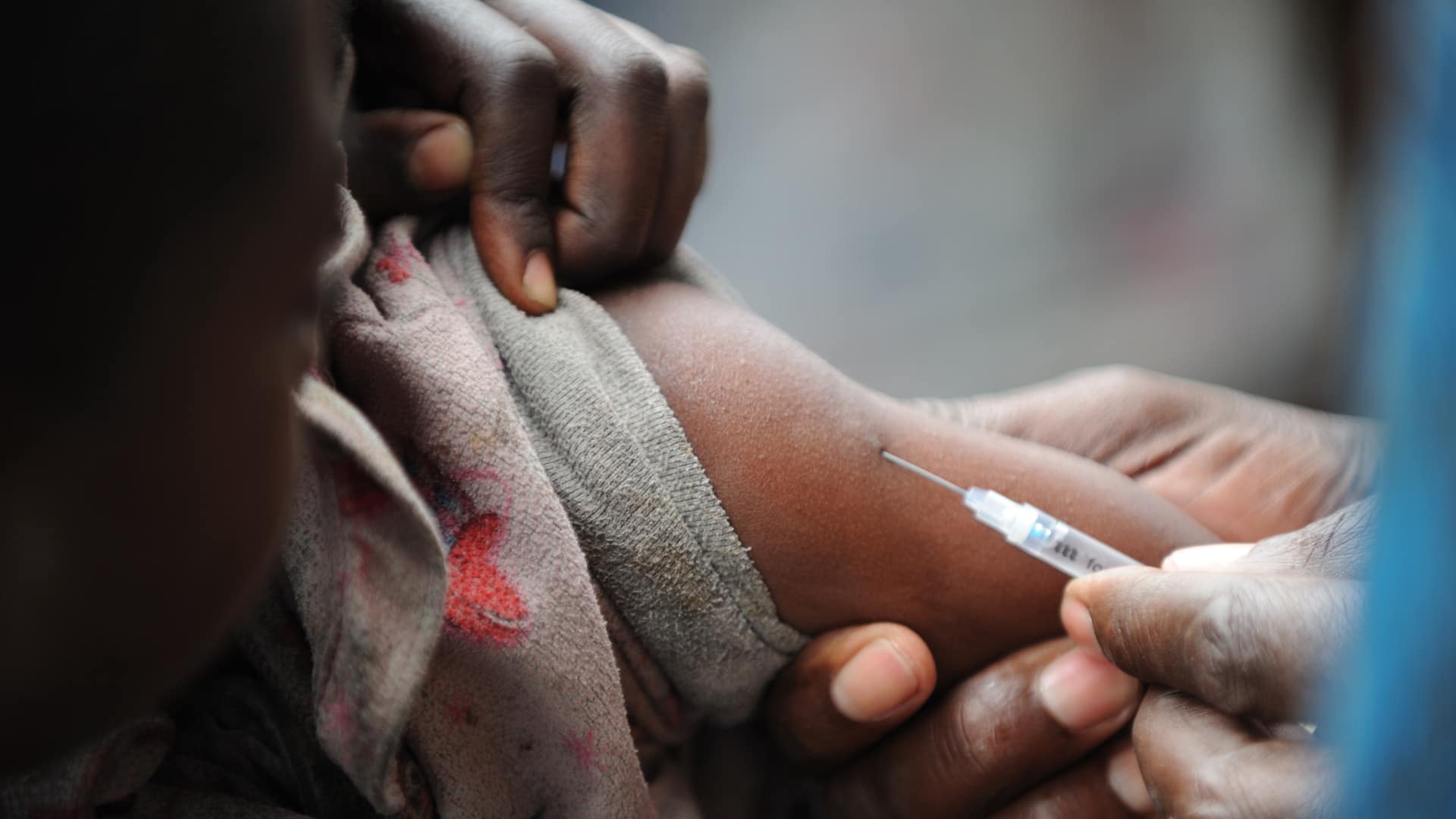
In Poor Nations, a New Disease Stalls Efforts to Fight Old Ones
When Lori Sloate visited the Democratic Republic of the Congo in January, the number of people killed by a national measles outbreak had just surpassed 6,000. The vast majority were children under the age of five. “I find it crushing that so many die from something entirely preventable,” said Sloate, senior director of global health at the United Nations Foundation in Washington D.C. The outbreak, which was declared in mid -2019, stemmed from a confluence of factors in the DRC that had crippled immunization and other health care services: political instability, infrastructure issues, ongoing outbreaks of polio and other vaccine-preventable diseases, and an Ebola epidemic.
The measles outbreak had become one of the largest in any one country since a vaccine against the disease was introduced in the 1960s, and global health authorities responded last year with multiple vaccination efforts, including a massive measles immunization campaign from October through December. Sloate arrived in the DRC shortly after the completion of that campaign, and her job was to work with government officials and other partners to identify any remaining gaps. Another wave of measles immunizations was scheduled for March. The goal: to reach nearly 1.3 million children who had been left unvaccinated.
“That was meant to be rolled out,” said Sloate, “and then Covid happened.”
The emergence of Covid-19 has now derailed the measles eradication effort in the DRC, and it threatens similar campaigns aimed at tackling a host of old scourges ravaging low and middle-income countries: measles, polio, tetanus, diphtheria, meningitis, typhoid, and yellow fever, among others. At least 25 countries have so far decided to suspend their campaigns, and more than 13 million children have already missed out on potentially life-saving vaccinations. Uganda, for example, postponed a preventative yellow fever campaign that had been set for April. Some districts in the DRC are continuing with mop-up measles campaigns; others have put those plans on pause.
These mass immunization campaigns, which usually involve workers going door-to-door, are supplemental to the routine vaccinations provided at clinics. But even routine vaccinations are now being hindered by disruptions related to Covid-19 — from breaks in the vaccine supply chain due to trade and travel restrictions, social distancing measures that keep families from accessing health centers, and concerns over exposing health care workers who are sorely needed to help fight the Covid-19 pandemic.
The feared fallout of all of this: significant setbacks for eradication campaigns against polio and the further resurgence of other old killers. “We also worry about diseases that may make Covid-19 worse,” said Kathleen Neuzil, director of the University of Maryland School of Medicine’s Center for Vaccine Development and Global Health. “If children are missing the vaccine for childhood pneumonia, we could see more childhood pneumonia from both missing vaccines, and from Covid-19 increasing children’s susceptibility to the disease.”
Neuzil serves on the World Health Organization’s Strategic Advisory Group of Experts on Immunization, or SAGE, which issued interim guidelines on March 26 that recommended postponing all preventive mass vaccination campaigns.
“We absolutely must protect the health care workers in these low resource countries or we will have a big problem going forward,” she said. “If we have a huge spread of Covid, not only will we see disease and death among the general population, but it could also decimate our health care workforce — at which point even if we wanted to have mass campaigns, we are not going to have the resources to execute them.”
The first case of Covid-19 in the DRC was reported on March 10. The country now has more than 240 reported cases. A recent analysis by Gavi, The Vaccine Alliance — an international organization that helps improve access to vaccination in low-income countries — found that, without any mitigation strategies, Covid-19 could cause nearly 13 million deaths in the world’s 73 lowest-income countries. (According to the analysis, that number does not include “any additional deaths resulting from disruption to critical health services, like immunization programs.”) Yet Neuzil acknowledged what she called a “very delicate and difficult balance.” Without question, pausing mass immunizations is putting millions of children at greater risk of contracting other diseases, she noted. As of March 29, the measles outbreak in the DRC had escalated further and has now claimed the lives of more than 6,600 people, according to provisional data from the WHO. .
At the same time, Covid-19 is itself a potent and deadly contagion — and one for which there is no vaccine at all.
“We are in a tenuous position internationally with many of these highly transmissible diseases,” said Neuzil. “We worry when routine immunization rates go down, it doesn’t take long before we see cases rise.
“We can’t trade Covid deaths,” she added, “for deaths due to vaccine-preventable diseases.”
In October 2003, the Global Polio Eradication Initiative (GPEI) launched what they hoped to be the final offensive against polio. They had been waging the fight since the WHO launched the immunization program in 1988. At that time, polio was endemic in 125 countries.
The plan was to immunize more than 15 million children in west and central Africa. Nigeria, in particular, still had a high prevalence of the disease — accounting for 45 percent of polio cases worldwide. But rumors quickly surfaced that Nigeria’s polio vaccine was contaminated with anti-fertility, HIV, and cancerous agents. After a 15-month boycott of the vaccine, the country’s polio cases shot up. The country struggled to eradicate the disease, and passed polio across its borders to countries previously polio-free such as Chad, Ghana, and Togo.
Today, after regaining some ground through aggressive campaigns, polio remains at large in only three countries: Afghanistan, Pakistan, and Nigeria. Two of the three wild strains of polio have now been eradicated, although one wild strain, alongside isolated strains of vaccine-derived poliovirus, continue to circulate. (Most lower income countries immunize children with an oral polio vaccine that contains a weakened live virus. It causes a very mild case of the disease. Those who get the vaccine can then spread that mild infection to others, which helps to bolster herd immunity. But if there is too much of the vaccine-derived virus circulating in an area where immunity is low, the virus is able to persist long enough to mutate into a more virulent form that, like the wild type, can cause disease, even paralysis. (This is the version of polio that remains endemic in Nigeria today.)
“We are close to eradication,” said Rebecca Martin, director of the Center for Global Health at the U.S. CDC, a partner with GPEI, the polio initiative, “but at the same time face challenges that now will be magnified with the Covid-19 pandemic.”
On March 24, two days before the WHO’s advisory group issued their guidance, the polio initiative made the call to suspend polio vaccination campaigns. They would devote the program’s infrastructure built up over the last 30 years — laboratory services, the transport of specimens, disease surveillance, contact tracing, and follow up — to help stop the spread of Covid-19. “It wasn’t an easy decision to come to,” said Martin.
Kim Thompson, president of Kid Risk Inc., a nonprofit research organization that specializes in integrated policy, risk, economic, and infectious disease modeling, is among scientists working with the WHO to model the impact of Covid-19 on outbreaks of vaccine-preventable diseases. The timing was particularly poor, she suggested, as the polio eradication program was already starting to lose ground. Case counts had jumped again in 2019. “Right now, I’m worried that this disruption might derail the whole thing,” she said.
“In order to achieve eradication we need to keep immunity really high,” added Thompson, noting the implications for both wild and vaccine-derived infections. “We need to make sure that any viruses circulating don’t have anywhere to go — that there’s not enough susceptible people.”
The battle against polio is further complicated by the fact that most people infected by the virus never show symptoms yet can still spread the disease, similar to Covid-19. (Also, as with the new coronavirus, treatment often involves a type of ventilator. Polio attacks the central nervous system so chest muscles needed for breathing don’t function.)
Measles, on the other hand, is generally considered a canary in the coal mine. Because of its high rate of infectiousness, and its obvious symptoms such as fever and rash, it is usually the first vaccine-preventable disease to show up when overall vaccination rates start slipping. “We are going to see a lot more measles cases first,” said Thompson.
 |
Thoughts or questions on Covid-19? |
This is true even though just two doses of a safe and effective vaccine can prevent measles. Between 2000 and 2018, measles vaccination prevented an estimated 23 million deaths around the world, according to the WHO. But again, because the virus is so contagious, approximately 95 percent of a population needs to be fully immunized to keep measles at bay and protect those left unvaccinated. In the DRC, only 57 percent of children received even a single dose of measles vaccine in 2018. That created ideal conditions to ignite an outbreak.
So far, 24 countries have suspended measles immunization campaigns as they cope with Covid-19. Global health organizations predict that more than 117 million children in 37 countries may eventually miss measles vaccines due to the pandemic. “It doesn’t take many children being missed before you can start to see measles outbreaks,” said Neuzil.
Measles, which remains a leading cause of death among children around the world, is especially deadly for malnourished children. Food insecurity is already an issue in lower income countries, and will likely be exacerbated by the Covid-19 pandemic. An April report from the World Food Program suggested that Covid-19-related containment measures may disrupt food supply chains, with potentially long-term consequences for low-income countries.
“I think we’re seeing wide-ranging impacts of this pandemic that probably weren’t anticipated,” said
Diana Chang Blanc, who coordinates immunization campaigns for the WHO.
On April 10, two days short of when the WHO was expected to officially declare the end of the DRC’s 20-month-long Ebola outbreak, a new case of the disease was logged. The country had gone 52 days without any reported cases. And as the world has been reminded with the spread of Covid-19, experts note, just one infected person is capable of igniting — or reigniting — an outbreak. This is among many factors that have made it difficult to forecast just how long the virus may continue to circulate and when measures to limit the spread, such as socially distancing and suspending immunization programs, might be safely loosened.
“If a shutdown lasts for a couple weeks or even a month, then countries can think through how to catch up and capture children that may have missed a dose,” said Neuzil. “But if it goes any longer, then we really start to worry.”
Understanding the complex dynamics of previous immunization disruptions and subsequent spreads of vaccine-preventable disease, such as in the DRC and Nigeria, could help modelers forecast the impact of current campaign interruptions, whatever their extent and duration. “We are in unprecedented times,” said the CDC’s Martin. “But we can use those data in models to predict what things will look like, and what is needed when thinking about recovery.”
Social distancing measures put in place for Covid-19 will reduce the risk of infection for other diseases, too. “But once that is lifted, those risks will go up immediately,” said Thompson, whose modeling will look at how best to mobilize immunization and other health care resources after the pandemic’s end to make up for lost time.
“The ideal thing is to get out with vaccines before you lift the measures,” she said.
Despite the disruptions to polio campaigns, GPEI is continuing to monitor the chain of production of polio vaccine, as well as the development of a new vaccine that they hope will be distributed later in 2020. The novel oral polio vaccine is more genetically stable — and hopefully less prone to sparking vaccine-derived poliovirus outbreaks — than the current version.
Meanwhile, global health experts urge countries to do what they can to maintain routine immunization programs. Doing so safely in the time of Covid-19 might entail efforts to reduce crowding in clinics, such as offering immunizations more days of the week, providing multiple public health interventions during a single visit, prioritizing the most vulnerable, and using individual rooms for vaccinations that were previously designated for nonessential services. “Spread people out, and make sure they wear masks and gloves,” said Neuzil. Yet she lamented that personal protective equipment, in addition to working sinks, soap and hand sanitizer, is often lacking.
“In the situation where countries are obligated to suspend their services or reduce their services, they should have strategies in place so that they can come back resolutely and quickly with the immunization programs once the situation permits,” added Chang Blanc. “If we’re successful in having a Covid-19 vaccine, this immunization system structure would help deliver those vaccines to those in need, too.”
In about a year and a half, global health experts anticipate that Covid-19 will become a vaccine-preventable disease. Ebola is a recent addition to that lineup, too, with an approved vaccine now licensed in multiple countries including the DRC. Better yet, though, would have been for the world to have stopped Ebola and Covid-19 before they took hold and joined this list of scourges that tend to disproportionately penetrate and pile up in the poorest countries.
“When the first SARS emerged, we eradicated it. It never got out of being an emerging disease,” said Thompson. “We should’ve shut this one down. And we didn’t.”