Nurturing Controversy: The Real Science Behind the Artificial Womb
Earlier this year, researchers at Children’s Hospital of Philadelphia (CHOP) revealed that they had developed an artificial womb capable of sustaining a premature lamb during a period of development roughly equivalent to 23 to 24 weeks’ gestation in humans. That’s a critical time. In the United States, an estimated 30,000 babies are born extremely premature each year. Weighing about one pound, their survival is uncertain. Those who do survive have a much higher likelihood of lifelong health problems such as lung disease, cerebral palsy, and hearing and vision impairments.
The new device, the researchers suggested, could one day dramatically improve outcomes for this particularly vulnerable group.
Such were the very narrow and targeted goals of the CHOP team. The public response among bioethicists and the media, however, was far more elaborate. In the weeks following the paper’s publication, a wide range of speculative narratives painted the development with a dystopian air. In an interview with NPR, Dena Davis, a bioethicist at Lehigh University, invoked Aldous Huxley’s “Brave New World,” in which human conception and gestation occur entirely outside the body — a concept known as “ectogenesis” — under the control of an autocratic state. In that same NPR segment, Scott Gelfand, a bioethicist at Oklahoma State University, worried that employers could require female employees to use artificial wombs to avoid maternity leave.
The U.K.’s New Statesman magazine ran an article with the title “Artificial wombs are only three years away — how scared should women be?” The author provided a feminist perspective on the question of whether an artificial womb will make women obsolete. And an article from Gizmodo declared that the technology could threaten a woman’s right to an abortion. In response, the conservative National Review magazine accused the Gizmodo author of wanting “a constitutional right to a dead baby.”
Discussions about where technology is taking us are surely warranted, though in the case of artificial wombs, the publication of one scientific paper became an occasion for speculation that left the particulars of physiology — and technology — in the dust. For example, the structural integrity of tiny blood vessels, the physical limits of synthetic tubing, the complex molecular exchange between fetus and placenta, and the often-poor outcomes of premature infants (despite receiving today’s most cutting-edge interventions) all speak to the immeasurably complex science attending fetal viability outside the human womb. Furthermore, the sometimes-sci-fi speculation potentially distracts from the murky ethical terrain that already exists in neonatal intensive care units across the country, where parents and physicians face a vexing question: Should they resuscitate an extremely premature infant with a high likelihood of death and severe disability?
A handful of groups worldwide are working on devices that would allow infants at this tenuous threshold of viability to survive. I became aware of the media conjecture while writing an article for the University of Michigan, where researchers are working to develop an artificial placenta. In the press, the lead researchers at CHOP and the University of Michigan have commented — not always favorably — on each other’s devices. But one thing both agree on: They are not trying to lower the age of viability, which is currently around 22 to 24 weeks’ gestation.
Dr. Alan Flake, a fetal surgeon and the corresponding author for CHOP’s Nature Communications paper, suggests that the ethical objections appearing in the press reflect a “lack of insight into the clinical context and the science that we’re doing.” Speaking about bioethicists in particular, he says, “It would be nice if they even just wanted to call me up and we could discuss it. It might add to their insight before they start raising these highly sensationalistic ethical objections.”
I. Glenn Cohen, a bioethicist and legal scholar, offers a different take. In an email interview, he writes that by staying ahead of the science — contemplating its possible trajectory and consequences — bioethicists can motivate the scientific community, laypeople, or legislators to change direction. “In my view,” Cohen says, “this is one of the most important contributions bioethicists make.”
While not completely discounting the thought experiments that accompanied the CHOP announcement (and which have followed analogous efforts elsewhere), a variety of scientists and medical practitioners suggest that the challenges and limits of technology are too often being overlooked. For anyone agonizing over (or hoping for) an imminent “Brave New World,” the scientific realities are likely to prove eye opening.
It’s worth noting that the term “artificial womb” never appears in CHOP’s research paper. The text, which describes how eight premature lambs survived four weeks without breathing air through their lungs, uses terms like “system” and “device.”
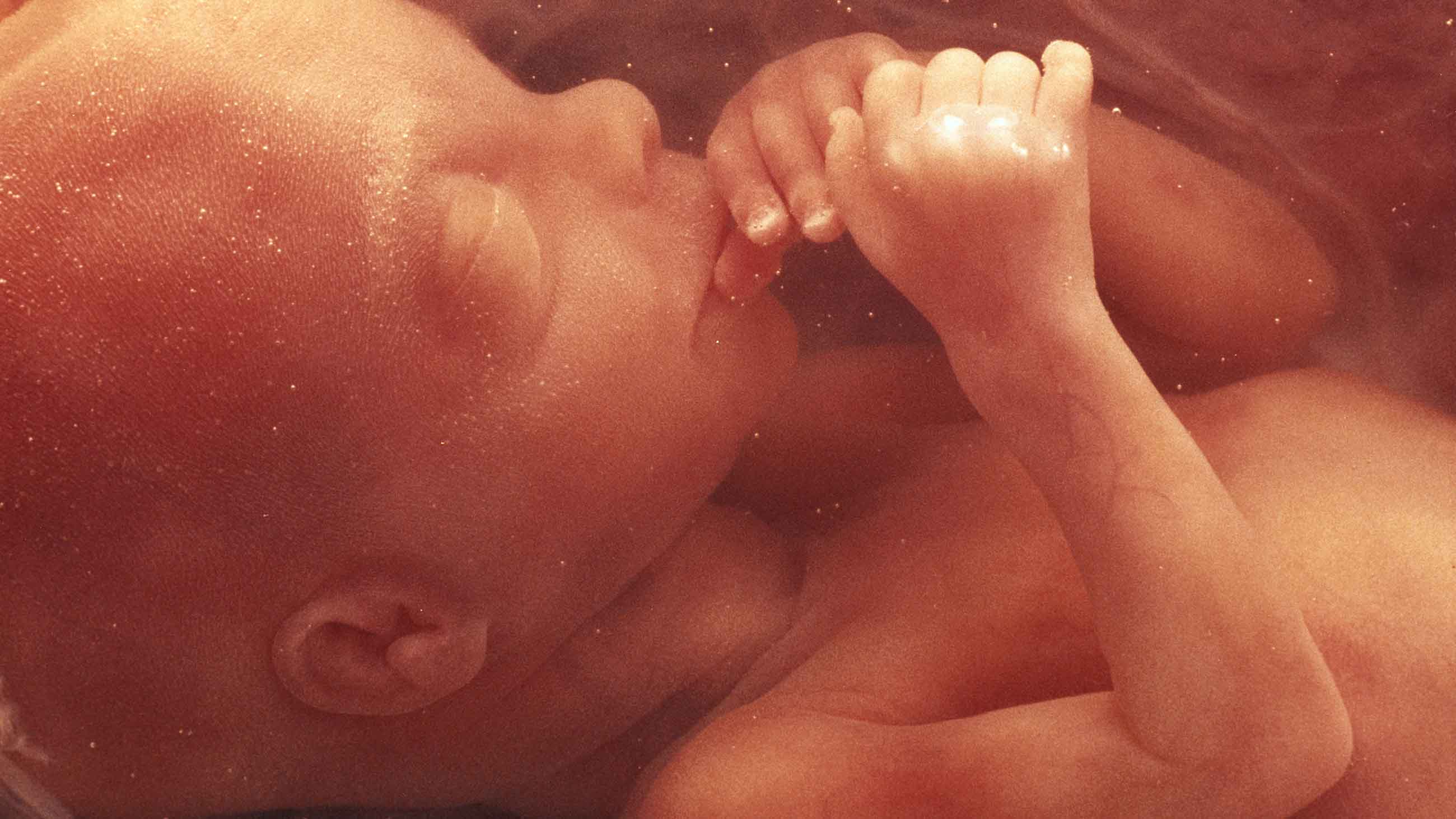
In photographs, that device appears otherworldly: A lamb is sealed inside a clear bag filled with synthetic amniotic fluid. Three small tubes, called cannulas, connect the umbilical cord to an oxygenator located outside of the bag, creating a circuit. Blood flows through the tubing from the lamb to the oxygenator, which provides nutrients and oxygen, while removing carbon dioxide. The replenished blood then flows back to the lamb.
In July, the Hastings Center, a bioethics research institute in Garrison, New York, provided a shot of adrenalin to the abortion debate when it published a report by Cohen that imagines a scenario in which an infant could be sustained in an artificial womb at 18 weeks’ gestation. That’s a tiny being, just over four months into a pregnancy and less than half a pound. Such a device, Cohen suggested, might lead courts to ban abortion at that age.
What would happen if doctors tried to connect this infant to CHOP’s artificial womb? There’s a vast difference in size and development between an 18-week-gestation fetus and a 23-week-gestation fetus, says Flake. The size difference matters because a smaller infant doesn’t pump as much blood. If there isn’t enough blood flow through the artificial womb’s tubing, the blood will clot. “At the present time, there’s nothing made or manufactured that can function adequately with those [lower] blood flows,” says Flake.
Even if a device could support a lower blood flow, it would be impossible to connect it to such a small infant, says Jutta Arens, a biomedical engineer working on artificial placenta technology at RWTH Aachen University in Germany. An artificial womb’s cannulas must connect with an infant’s blood vessels, but the smaller the baby, the smaller its vessels. If the blood vessels aren’t thick enough, they won’t be able to stabilize a cannula. “There really is a physical limit to everything that we do regarding the diameter of the vessels of the baby,” she says. The German group’s current target is 24 weeks’ gestation. “Perhaps we could go down to 23 or 22,” she says, but “I don’t think we could push the limits further down.”
Similar devices already exist that take over heart and lung function for adults and children recovering from organ failure. But they are only a last resort because complications can arise from long-term use. These technologies save thousands of lives, but their effectiveness is time-limited. This is one of the reasons Flake considers it “very unlikely” that a device like his could support an infant as long as 5 or 6 weeks.
“We’re trying to optimize the benefit-to-risk ratio here,” says Flake. “By going back to 18 weeks, you increase the risks dramatically and really negate the benefit.” I sense that Flake is tiring of these hypotheticals, but I press on: What about speculation that artificial wombs could provide a desirable alternative to pregnancy?
“That’s all pure fantasy stuff,” he says. “They’re making this stuff up just for the sensationalist value of it. It’s ridiculous. You’re never going to have a zero-risk system.”
Artificial wombs and placentas are being developed with the goal of treating infants who are already receiving intensive care in NICUs across the country.
“In the United States, children born at 23 or 24 weeks’ gestation — most of them are going to receive attempts at aggressive care,” says Dr. Mark Mercurio, chief of neonatology and director of the program for biomedical ethics at Yale School of Medicine. This includes measures such as mechanical ventilation, fluid and electrolyte management, and surgical procedures.
Despite these interventions, outcomes for this group of infants are so poor that they exist in what’s called the “gray zone” of viability, when survival is uncertain and chances of severe disability are high. Among infants born at 23 weeks’ gestation, only about a third survive. At 24 weeks, the odds of survival double. Among survivors in both groups, the likelihood of disability is extremely high due to long-term health issues such as chronic lung disease, neurodevelopmental problems, and impairments of hearing and vision.
Mercurio believes a technology that improves outcomes for these children “would receive a great deal of interest.” He sees that as a better focus than the question, “Couldn’t we get them even smaller?”
Sandra Bellini, director of the Neonatal Nurse Practitioner Track at the University of Connecticut School of Nursing, has spent 30 years working in neonatal intensive care. She is skeptical about the notion of lowering the current age of viability because while neonatology has made great strides in treating premature infants, “every single thing we do can carry risks of short- and long-term damage” to the baby. “We are all about saving babies, but we want to save babies who are going to go on to have a happy, healthy life,” Bellini says. She mentions data showing that families whose babies received a high degree of medical intervention in the NICU have “huge incidences of [post-traumatic stress disorder], divorce, and financial ruin.” Some families have medical insurance policies with a lifetime cap. Daily NICU costs exceed $3,000 per infant, and a prolonged stay can top one million dollars. NICU children can hit their cap before they ever leave the hospital.
All of this means that parents of infants born at 23 weeks’ gestation must make a difficult decision about whether to pursue aggressive, uncomfortable, and often ineffective care for their premature baby. A successful artificial placenta, by improving outcomes for these infants, would eliminate the decision. “My device doesn’t introduce huge ethical questions if it’s applied appropriately, meaning to a 23-weeker to improve outcome,” says Flake.
For its part, the CHOP team is not against bioethical input on these technologies. In fact, they’re collaborating with some bioethicists to identify the best way to introduce artificial wombs into the clinic once the technology is ready. Describing his artificial womb, Flake says, “I think it needs an ethical framework that is based on its capabilities and the science and the clinical context that it will be used in.”
Even if CHOP’s artificial womb isn’t capable of lowering the current age of viability, isn’t it possible that once in place, it might allow other research groups to create a device that could?
“Not a chance, no. Not good,” says D. Michael Nelson, an obstetrician at Washington University School of Medicine in St. Louis, who has been researching the placenta for over 30 years. He is editor emeritus of the journal Placenta, and recently gave an inaugural address at the International Federation of Placenta Associations.
“There are a lot of programming things that go into babies,” he explains. In this case, he isn’t referring to genetic programming, but to programming that comes from interactions with the environment to which the baby is exposed in the mother’s womb. The maternal placenta provides a complex and changing mixture of proteins, lipids, carbohydrates, minerals and growth factors. “You start putting [babies] in an artificial environment, and it changes everything,” says Nelson. Machines and artificial sources of nutrition are not as good as the placenta and the mother’s blood supply.
Nelson believes that researchers will make significant advances in prematurity prevention before they perfect an artificial womb. He cites research at the March of Dimes Prematurity Research Centers, a network of researchers based at major medical centers, including his own, studying how factors such as the microbiome, circadian rhythms, and genes might contribute to prematurity.
“Our goal is to avoid premature birth,” he adds in an email message, “rather than putting our preterm babies in a bag.”
That’s certainly a brusque way to describe the technological advances being made at the frontiers of infant viability. But in its brusqueness, it also serves to underscore the vast distance between the science of human gestation as it now stands, and the faraway horizons where it would need to go to breathe real life into the ethical worries — boxed pregnancies, valueless women, and other Brave New Worlds — that the CHOP innovation recently set in motion.
Of course, to bioethicists, the gap between what we can do now and what we might be able to do in the future is precisely where all the potential consequences ought to be fully considered. “By the time a breakthrough is here and widespread,” Cohen says, “it is often hard to have a real conversation about ‘where to go’ because we are already there.”
By most measures, scientists suggest, we won’t be there for quite some time.
“Reproduction is very complex and it’s taken millions and millions of years to create the systems we have and there are still huge amounts that we just don’t understand about it all,” says Dr. David Adamson, a reproductive endocrinologist and CEO of Advanced Reproductive Care, a national network of fertility clinics.
Adamson believes that ectogenesis might one day be possible, but in the distant future: decades at least, perhaps even a century. He also points out that this will likely require technologies other than those currently available to us. He mentions big data, and a better understanding of gene expression, and perhaps stem cells to create special types of placental tissues that aren’t currently available. “If we look over 40 years, because IVF’s not 40 years old yet, we see that there’s been a lot of progress in terms of our being able to do in vitro growth of embryos on the one hand, and, on the other side, to reduce the gestational period at which viability can occur,” he says.
But just as IVF and surrogacy are supplemental procedures today, he envisions ectogenesis as an assisted reproductive technology, akin to IVF but much more complex — and far, far in the future.
In the meantime, many scientists agree with Jutta Arens, the German engineer:
“There’s no way,” she told me, “of substituting the womb.”
Sara Talpos is a freelance writer whose recent work has been published in Mosaic and the Kenyon Review’s special issue on science writing. Sara has an MFA in creative writing (poetry) and is interested in the connections between science and literature. She taught writing classes at the University of Michigan for ten years.










Comments are automatically closed one year after article publication. Archived comments are below.
I would love to try I got remarried I would love to be able to have his children but I can’t I had a Partial history can you 5 years ago I would do anything to have a baby now
There is no definitive proof that an artificial womb will never be able to replicate a natural womb. Admittedly, it could be many centuries in the future, but “never” is a strong word, especially in science. It is foolish to assume that the technology will advance no further.
bioethicists are the new Luddites
Artificial Womb will also end the Abortion Controversy. Theoretically, as the technology improves, all the aborted babies will be should be able to survive without their mothers. But it will drive up the price of abortions when the cost of the Artificial Womb and Child Support are factored into the equation.
You clearly explained the very reason the contraversy will in fact not end that day. As long as self-aware humans are around, there probably has been the need for arbortions. If the legal procedure is to expensive and connected to livelong obligations (the mental stuff aside), desparate women will look after unsafe amateur stuff instead. A possible way to relieve society of dead unwanted babies could be education (to avoid unwanted pregnancies in the first place). And the only way to save women from bleeding to death or die of some serious infections contracted in some dark chamber, is maybe the possibility to get a affordable safe procedure, under clear ethical approved rules. Supported by a society that hopefully does not condemn women in extremely demanding psycho-physical conditions.
Judging by your spelling, grammar and punctuation I hope you just made up the name “med schooler”. There is no way you are a high school graduate.
I had a 24 weeker almost 2 years ago. The first month of his life was a roller coaster. Care was extremely aggressive. Even with excellent care he caught 3 infections simultaneously and one of them infiltrated his spinal fluid. We had a very good outcome because he only developed retinopathy and minor lung trouble. I’m glad that researchers are trying to develop a system to improve the outcome for micropreemies. I guess the people who object have no idea what reality is like for extremely premature babies. I certainly had no idea before having one.