For Childhood Ear Infections, Ear Tubes May Be Overprescribed
When a child gets an ear infection, it can be agony for the whole family. Prasanth Pattisapu knows this firsthand — he’s a father and a pediatric ear, nose, and throat doctor at Nationwide Children’s Hospital and professor at The Ohio State University. During his daughter’s four ear infections, he said, “she was not sleeping, just screaming in pain.”
Ear infections are a common childhood diagnosis, and doctors usually either wait to see if they clear up without intervention or treat them with antibiotics. But every year, about half a million children in the United States undergo a more invasive treatment for frequent ear infections or persistent fluid in the middle ear: tympanostomy tubes, or ear tubes. Doctors surgically insert these tubes into the ear drums to help equalize pressure between the ear canal and the middle ear. It’s one of the most common outpatient surgeries performed on children in the United States.
Whether all those procedures are warranted, though, is up for debate. Ear tubes aren’t without risks, from bleeding to scarring to infection. And some research indicates that the procedure might not work better than less invasive alternatives. Given the difficulty examining the inner ear, some experts have also suggested that ailing children are sometimes diagnosed with ear infections even when no infection is present.
Citing concerns over the overuse of ear tube procedures, the American Academy of Otolaryngology published new ear tube guidelines for children in 2013. These were updated again in updated in 2022 to help providers determine when a patient will benefit from ear tubes. The current criteria, though, are “based on well-documented ear infections,” Pattisapu said. “But in truth, we rarely get well-documented ear infections.”
And yet, identifying a true ear infection can be tough for providers. “We know that ear infections are not always diagnosed accurately in primary care. There tends to be overdiagnosis,” said Richard Rosenfeld, an otolaryngologist (another term for an ear nose and throat, or ENT, doctor) and distinguished professor at SUNY Downstate, who co-authored the AAO guidelines. For primary care providers, diagnosis often relies on subjective interpretation of symptoms, and the inside of the ear can be hard to see and fully assess. And when a child has multiple ear infections, they are referred to a specialist who relies heavily on primary care providers’ past diagnoses.
Ideally, Pattisapu said, providers would have a more objective way to diagnose ear infections in the first place. It’s a problem that other experts are working to solve with solutions that include an smartphone app to diagnose the infections, and a device that can automatically detect ear conditions. “What would be great,” he added, “is if we had a perfect way of diagnosing an ear infection in the hands of every pediatrician in every clinic in the country.”
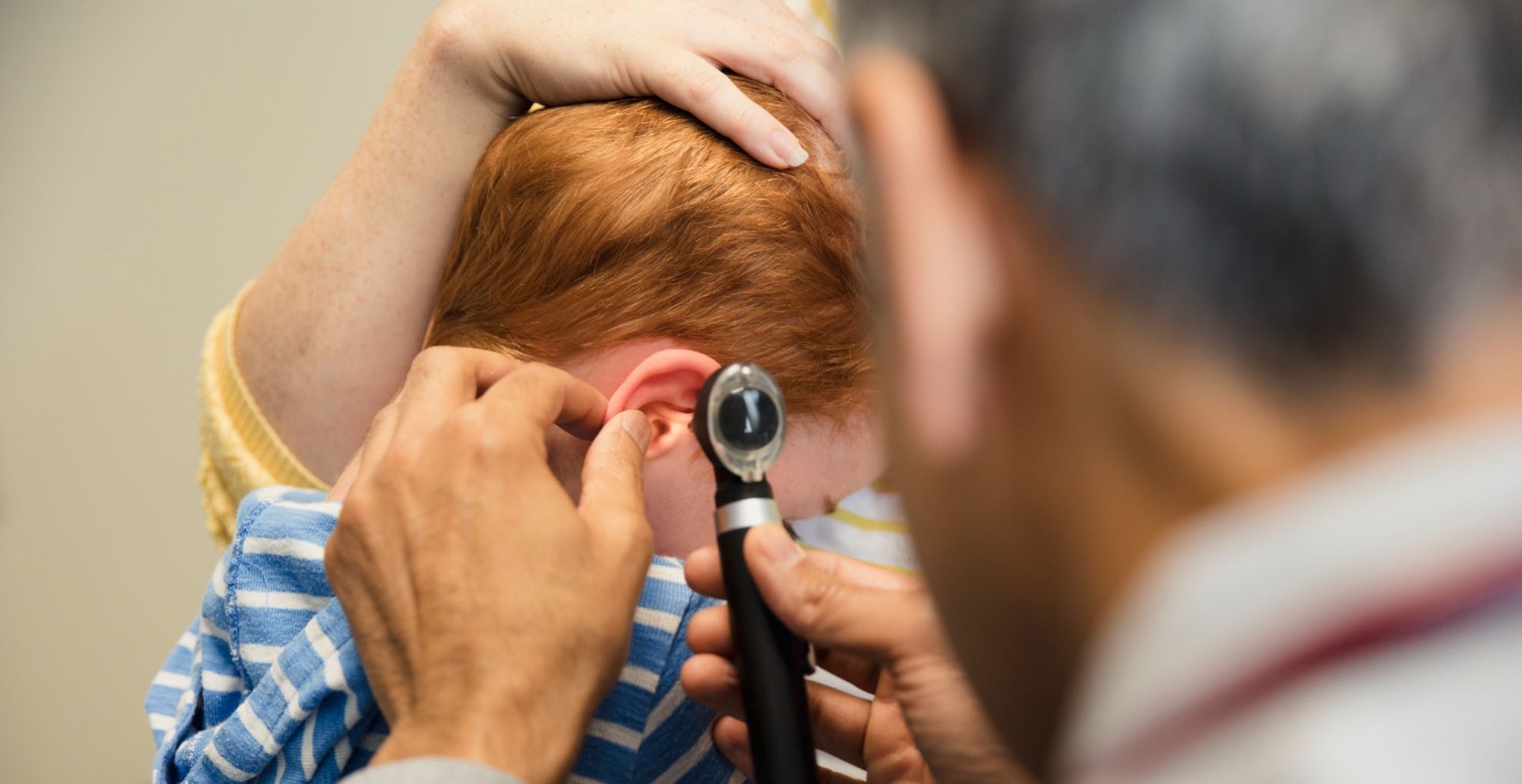
In children, a typical ear infection diagnosis begins with a health care provider determining whether the child has a bulging ear drum. But looking deep into the ear to see the ear drum, let alone concluding that it is bulging, can be challenging. For one thing, earwax gets in the way, Pattisapu noted. Children also tend to be sick and miserable when they visit a pediatrician. They may have a fever, or just cry or scream, all of which can also make the eardrum turn red and possibly bulge — even when no infection is involved.
If a provider sees a bulging ear drum, they may prescribe antibiotics, though the American Academy of Pediatrics recommends watchful waiting for many cases.
But frequent antibiotic use may have negative consequences. Antibiotics can wreak havoc on the microbiome, Rosenfeld said, and “we’re just starting to understand this balance of bacteria on health in general.” Studies suggest that antibiotic use early in childhood is linked to allergies, asthma, obesity, developmental disorders, and more. (It’s not yet clear whether antibiotic use is the cause of those health problems, or children who receive antibiotics were already more prone to those outcomes.)
According to the AAO guidelines, ear tubes are an option after a child has four ear infections within one year — including one in last six months — or three within any six month period. They should also have some fluid in the ear at the time the child is seen by an ENT, according to the guidelines, because “we know from research studies that kids who don’t have fluid in their ears but have frequent ear infections tend to get better” on their own, Rosenfeld said. The fluid also indicates that at least the most recent ear infection was diagnosed accurately, he added.
To insert an ear tube, an anesthesiologist sedates the child, then an otolaryngologist cuts a small hole in the ear drum, and then slides in a tiny plastic tube that is roughly the size of the point of a click-top pen.
Ear tubes have upsides, according to some experts. For instance, Pattisapu said ear tubes allow for a more direct application of antibiotics. The drugs are usually given orally, which can cause diarrhea and may be associated with other negative health outcomes. With ear tubes, antibiotic drops can be applied directly to the ear. (An ongoing clinical trial is investigating whether the drops can treat ear infections even without ear tubes.)
Some experts also stress that ear tubes help avoid hearing loss due to fluid build-up, although the evidence on this is mixed, Pattisapu said. A 2017 review of 147 research articles on tympanostomy tubes indicated a short-term improvement in hearing at 1 to 3 months post-procedure, but no benefit one year later, compared to holding off on the surgery. (Rosenfeld says children with developmental delays may benefit from the short-term improvement in hearing.)
Still, ear infections are possible even with the procedure, and may still require oral antibiotics. Additionally, studies suggest there are fewer infections in the first year after ear tube placement, but by the second year there may be just as many ear infections and oral antibiotics prescribed to those with ear tubes compared to those without. Desmond Nunez, a pediatric ear, nose, and throat surgeon at the University of British Columbia who authored a 2018 review of evidence, suggested that studies indicate ear tubes lead to about one less ear infection in a six month period, with a less noticeable effect after a year.
And for recurring ear infections, there’s growing evidence that ear tubes may not be better than oral antibiotics. Alejandro Hoberman, a pediatrician and pediatrics professor at the University of Pittsburgh School of Medicine who led a randomized trial of ear tubes versus oral antibiotics in 2021, said the main benefit of ear tubes “was it delayed the first-year infection by two months.” While the researchers also found that the duration of ear infections was slightly less in patients who got ear tubes, the overall rate of subsequent ear infections was not significantly different compared to those who got oral antibiotics over a two-year period. Rosenfeld, who was not involved in the research, said the study indicates that either ear tubes or antibiotics are acceptable ways to treat recurrent ear infections. (Hoberman is named on a patent for a pediatric oral antibiotic suspension licensed by the University of Pittsburgh to Kaizen Biosciences, where he also serves as a board adviser.)
Although earlier data supported ear tubes in favor of antibiotics, the studies were published before the development of vaccines that included certain strains of pneumococcal bacteria, which are a cause of many ear infections. “The vaccines overall have some effect in reducing the need for ear tubes,” Rosenfeld said.
Nunez also points out that since the mid-2000s, there have been few robust studies on ear tubes compared to other treatments.
Ear tubes also come with risks, though they are rare, Rosenfeld said. Between 1 to 2 percent of patients end up with a small hole in their eardrum that needs repairing, and 5 percent will continue to have recurrent ear infections. Occasional drainage from the ear — a clear, mucousy or pus-like discharge — is also common. Ear tubes may also increase the likelihood of subsequent surgery; one study suggested that about a quarter of children who had the procedure needed a second placement.
Despite the downsides, according to Rosenfeld and Pattisapu, if the clinical guidelines are met, the benefits from ear tubes may outweigh the risks. And a 2019 study indicated that the guidelines are effective at preventing unnecessary ear tubes — most of the children who held off on the procedure, per the guidelines criteria, didn’t need ear tubes. But Nunez said that there needs to be more clinical trials to know for sure that ear tubes really are the best treatment option for recurrent ear infections.
Ear tube surgeries also may not always happen for the right reason, and some evidence suggests economic disparities among the patients who receive them. One 2019 study published in the Journal of Pediatrics by researchers at Nationwide Children’s Hospital, for instance, indicated that zip codes with the most privately-owned outpatient surgery centers perform 52 percent more ear tube procedures than surrounding areas, adjusting for population. Additionally, the vast majority of ear tube patients are White and more than two-thirds have private insurance.
There may also be other motivation for some doctors to guide parents toward surgery. Nunez pointed out that some countries have higher rates of ear tubes than others, without any evidence of higher rates of ear infections or other disparities to account for differences. For instance, he said, the United Kingdom has much higher rates of ear tubes than the Netherlands. “Some of it has to do with incentives,” he said, noting for example, that in the U.S., both the hospital systems and the clinician receive revenue from interventions. This results in “a system that’s going to lean towards intervention,” Nunez argued.
But he also attributes it to “the culture of medicine or the way medicine is practiced” in different countries, which is partly clinicians’ decisions, and partly expectations of parents for how recurrent ear infections are managed. He said that in comparing treatment options, “the differences are probably at the margins.”
While financial incentives might drive some providers to place ear tubes, those who are in an academic setting, like a hospital, are “a bit distant from that,” said Pattisapu, who added that he is more troubled about patients who don’t have equitable access to health care than he is about overuse.
Fortunately for Pattisapu’s family, his daughter hasn’t had another ear infection. However, because he is sure of her diagnoses, if she had another he would have taken her to get ear tubes. He personally would choose the procedure over more rounds of oral antibiotics, but, he said, based on the current evidence, “you have to make it a very personal decision.”
Christina Szalinski is a freelance science writer with a Ph.D. in cell biology based near Philadelphia.












Comments are automatically closed one year after article publication. Archived comments are below.
I am a pediatric ENT doc who also happens to repair eardrums and I agree with Dr Hoberman.The permanent damage to ears/hearing done by tubes is grossly understated and often misrepresented.
My son had ear tubes placed for recurrent ear infections when he was 2 (30 years ago). He had delayed speech development due to hearing loss attributed to frequent infections. It took years of speech therapy to recover, but without the ear tubes the damage could have been permanent.
Jeepers, I thought most proved to be kids gavaged rBGH (bovine somatotropin) with a typical US, HFCS & GE Monoculture/ CAFO toxic junk-food, killed-back with lethal herbicides, processed with any chemicals not in radium flavored fracking brine irrigating the dead, nutrient free soil pumped full of agricultural wastes?