To Treat Babies for Drug Withdrawal, Help Their Mothers, Too
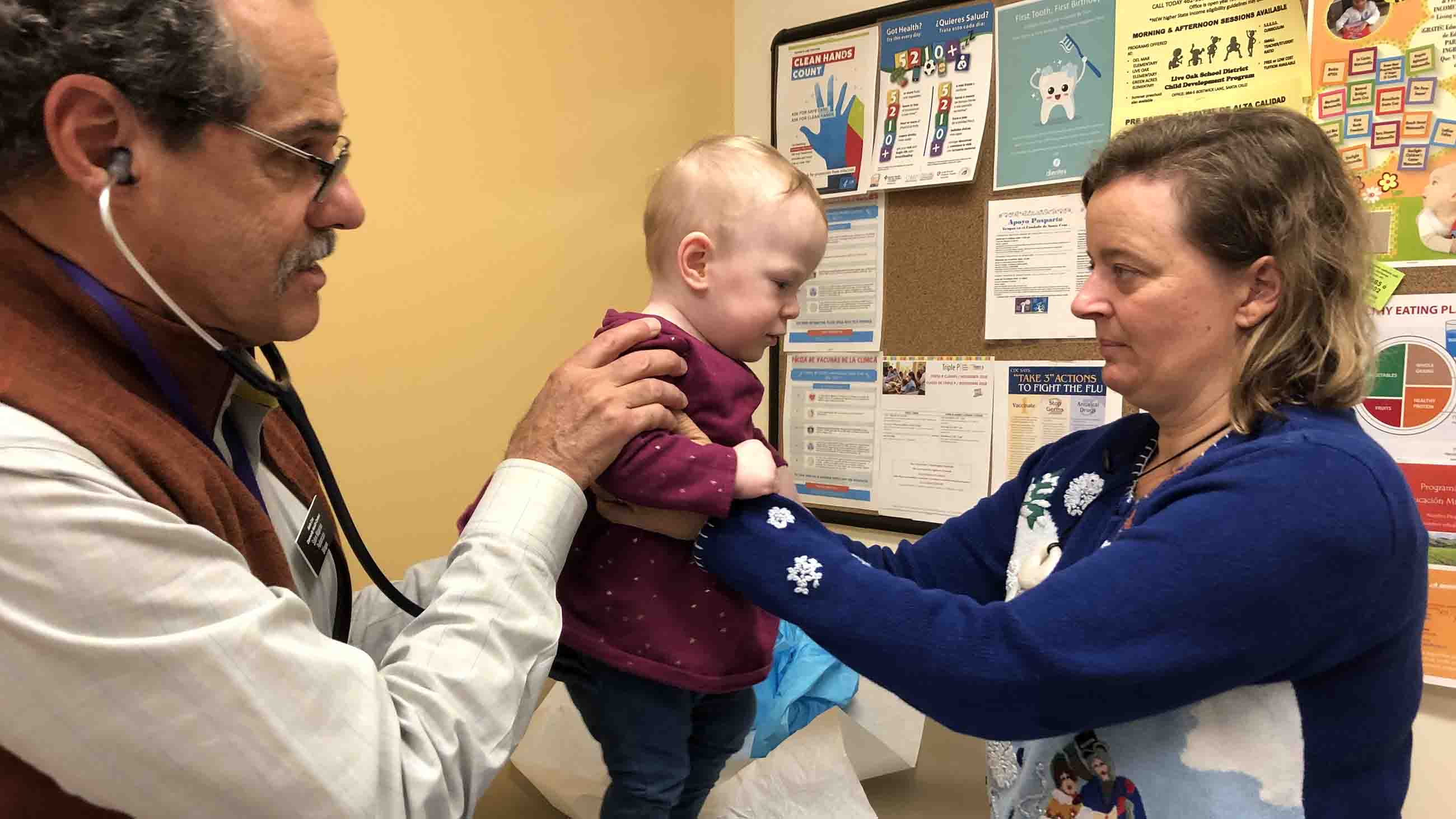
Six-week-old Jose Martinez Castillo stares up at his pediatrician and begins to scream. “I have a way with babies, don’t I?” Dr. Salem Magarian intones, grinning at the baby’s mother, Lisa Castillo, who is preparing a bottle of formula on the other side of the exam room.
Castillo, 39, watches as Magarian checks Jose’s reflexes and listens to his heart. The doctor places Jose back in Castillo’s arms. She nestles him against her pink blouse printed with “LOVE” in gold letters and sings quietly as she feeds him. The baby’s eyes gradually narrow to slits.
Already today, Magarian has seen more than half a dozen babies like Jose inside the brightly painted walls of the East Cliff Family Health Center, located in Santa Cruz, California, a few blocks from the shimmering Pacific. While this particular visit doesn’t stand out for him, it does for Castillo. She has given birth to five children during her two-decade struggle with heroin. Jose is the first one she’s been able to keep.
Born dependent on methadone, the boy arrived prematurely and spent two weeks in the hospital, his small body trembling and stiff from the pain of withdrawal. A week after he was discharged, he started choking while breastfeeding and Castillo rushed him to the emergency room. Today, though, Jose seems to be thriving.
Magarian, who has a gray horseshoe moustache and an easy smile, has cared for more than 300 babies born with neonatal abstinence syndrome (NAS). Over the past decade and a half, he and his colleagues have developed a system that, at its heart, aims to support babies and their mothers, who frequently struggle with addiction, trauma, and the stigma of birthing a baby with NAS. This approach is part of a growing movement that recognizes the importance of mother-infant bonding for these vulnerable children. “Treat mom like she’s antibiotics for pneumonia,” explains physician Matt Grossman, who practices at Yale New Haven Children’s Hospital.
There’s a crucial need for new approaches. Nationwide, the number of mothers with an opioid use disorder at delivery more than quadrupled between 1999 and 2014. During roughly the same period, the number of babies born with NAS increased sevenfold. Today, one baby is born with NAS every 15 minutes. These babies are not considered “addicted” by experts because babies do not have the psychological profile that allows for addiction. But withdrawal in babies mimics withdrawal in adults: painful stomach cramps, vomiting, seizures, bodies so stiff it can be hard to change their diapers. Sometimes they struggle to eat or sleep and will scream inconsolably for hours.
These problems are compounded when babies and their mothers don’t receive proper care. Years ago, before Santa Cruz changed its system, nurses at Dominican Hospital — where Magarian worked until 2014 — sometimes didn’t know if a woman giving birth was using drugs, nor did they always recognize the signs of withdrawal. Some babies ended up going home without treatment or services, increasing their risk for seizures or Sudden Infant Death Syndrome. When nurses did identify babies with NAS, the infants were sent to the neonatal intensive care unit (NICU), where they would remain for two or three weeks. There, various doctors would experiment with different medications in the hopes of alleviating their symptoms.
Many of these babies were then placed directly into foster care, even if their mothers were in recovery. Since there weren’t enough foster families in the county to care for medically fragile babies, nurses sometimes ended up taking them home. Many pregnant women, afraid of having their babies taken away, either hid their addictions or left the county to give birth.
With relatively few federal or state guidelines to standardize care of these mothers and children, this pattern repeated itself at hospitals and clinics across the country. The collateral damage from all this confusion was, of course, the babies.
Today, doctors and nurses are experimenting with a variety of new, less intrusive methods for assisting mothers and their newborns confronting NAS. But just a short time ago, no one — Magarian included — knew the best way to help them.
“We were getting nowhere in terms of having a system,” Magarian said. “We didn’t have much, and what we had was not integrated, was not standardized, was not at all predictable.”
Historically, one major impediment to better care for babies with NAS has been the tendency to blame their mothers for using illegal substances while pregnant. Stephen Patrick, a neonatologist at Monroe Carell Jr. Children’s Hospital at Vanderbilt University, says that among people with substance use disorders, “There’s no population that’s more stigmatized than pregnant women.” He says there is a sense of, “How could you do this to your baby?”
Dr. Hendrée Jones, the executive director of the University of North Carolina Horizons Program — which offers mothers with substance use disorders intensive treatment, psychiatry, case management, therapy, and other services — agrees. There is a “tremendous amount of blaming and shaming and stigma,” she says. “Unfortunately, that is something that has not changed at all in the 25 years I’ve been in the field.” Too often, this stigma drives women from treatment. But having the mother on and off drugs is dangerous for fetuses. Staying stable on methadone or buprenorphine is much safer.
Still, these medications can cause babies to go through withdrawal. Even with supportive physicians, many mothers struggle with guilt. Kara Pardini was on methadone when she gave birth to her now-10-year-old son, a longtime patient of Magarian’s. He cried constantly and had the shakes. Pardini said that, unlike Magarian, some of the providers who cared for her and her son early on treated her with coldness.
“I would cry all the time,” she said. “I felt so guilty that I had him born on that medication.”
Lisa Castillo, Jose’s mother, has also struggled with this guilt. After Jose was born, he suffered from loose stools, watery eyes, tight muscles, and shaking and tremors.
“It was hard to watch it,” she said. “It’s not something I wanted him to go through.”
Magarian remembers the moment, back in 2004, when he realized how counterproductive it was to blame the mothers. That day, he was making rounds accompanied by nurses, a social worker, a pharmacist, a chaplain, a child welfare worker, and other colleagues. Their conversation turned to a four-day-old baby who had just had a seizure and was in withdrawal. Until then, no one had realized the baby’s mother was using heroin during the pregnancy, and at first, people were angrily venting their frustrations about the baby’s mother.
“Let’s stop for a second,” Magarian said. “Didn’t we have this exact same conversation — didn’t we say this exact thing — isn’t this a mother we had this same conversation about 24 months ago? What happened to that baby?”
Nobody knew.
Magarian and his team realized they needed to do more for both mothers and babies, but there wasn’t much in the scientific literature to guide them. “The county was in a pretty dire place,” said Susan True, who at the time was director of a county commission for young children called First Five. With the introduction of smokable heroin, or “chiva,” some women were becoming addicted without realizing what they were using.
“We were also feeling like ‘we can’t wait for an answer,’” True said. “‘We have a problem right now.’” So, over time, a multidisciplinary team based at Dominican and spearheaded by Magarian, developed a model with many prongs that involved agencies throughout the county.
Through a voluntary prenatal program, every pregnant woman could access home visits and drug and alcohol counseling without facing judgment or fear of repercussion. A social worker got to know mothers before they delivered, then walked down the hall to help support them while their babies were in the NICU. Nurses were trained to provide comfort care to babies going through withdrawal, to keep them in quiet rooms, to teach their mothers to swaddle them and hold them skin to skin.
Because so few doctors in the community were interested in working with babies with NAS, and because consistency of care seemed crucial, Magarian started working in the hospital’s outpatient clinic to see all babies born with NAS. The babies also received weekly occupational therapy and were referred for developmental assessment to the Stanford High-Risk Infant Follow-up Clinic, as well as other programs.
The team also developed a weaning protocol — every baby who exhibited signs of serious withdrawal was put on the same small dose of morphine, which increased up to a certain limit until the baby stabilized. Babies who were stable for 48 hours were sent home to wean. The team asked the head of child welfare to allow women in recovery to keep their babies.
Some county employees were initially skeptical about sending fragile babies home with mothers who had just gotten off of heroin — and then allowing those mothers to administer morphine themselves. But according to the team’s lead nurse, Chris Terry, none of the mothers ever drank their babies’ morphine. At any rate, it was too small a dose to have much of an effect, she said.
There hasn’t been a peer-reviewed investigation into the model developed in Santa Cruz. But the limited data Terry and others were able to collect seems to back up the approach, they say.
Nationally, babies with NAS tend to stay in the hospital an average of 3.5 times as long as most other newborns. Their care costs more than three times as much. After the county introduced its new program, stays in Dominican’s NICU dropped from 14 days to nine. Fewer babies landed back in the emergency room. More mothers stayed in long-term recovery.
The rate of child abuse appeared to drop as well. In 2005, when the program started, Santa Cruz County had 16 cases of substantiated child abuse per 1,000 children — well above the state average. By 2013, that had dropped to seven cases per 1,000 children. It has remained below the state average ever since.
“I really am struck by accomplishments like this,” said True. “Very, very few communities get population level change. It’s exciting to know that we did that in Santa Cruz.”
In this video overview of a 2018 paper published in the journal Pediatrics, researchers describe the increasing incidence and cost of neonatal abstinence syndrome (NAS).
These changes have made a huge difference in the lives of women like Lisa Castillo, who as a teenager, experienced trauma, developed depression, and started hanging with the wrong crowd. One day, she saw someone smoking something and asked if she could try it. She didn’t know heroin was addictive. She just wanted to feel better.
She got off drugs before giving birth to her first baby, at 20. Then she discovered her partner had cheated on her. Depressed, she sought solace in the familiar. Lost in a heroin fog, she didn’t realize she was pregnant with her second child until she was five months along. She tried to quit and went into withdrawal. She rushed to the emergency room, where a doctor told her withdrawal might lead her to miscarry. “His words were, ‘You’re better off using because you can miscarry if you don’t,’” she said. “I left the ER without any medication and went back to using and used through my whole pregnancy.”
Her daughter was born in the morning, and by 11 p.m. that same day, the infant was in state custody. Castillo went on to have two more children, whom she also lost custody of. Her parents are raising her four older children, so she is still able to see them.
But when Jose was born earlier this year, things were different. She takes not only methadone, but also Wellbutrin to help manage her depression, and she sees a therapist to help her navigate past trauma. More pointedly, rather than being separated after he was born, Castillo and Jose live together in a transitional home for women with new babies. They were referred by the local child welfare department to a voluntary, court-supervised treatment program and to a separate program for families with children affected by drugs. An instructor there is teaching her therapeutic exercises and massage to help relax Jose’s stiff muscles. Castillo says she can’t help but wonder what might have happened if she’d received these services when she was younger.
In 2016, President Barack Obama signed the Comprehensive Addiction and Recovery Act, which required individual states to outline requirements for the safety and wellbeing of infants affected by substance use, including the needs and treatment of their family members and caregivers.
Despite this, innovative, multidisciplinary efforts like Santa Cruz County’s remain relatively rare.
That said, a handful of noteworthy efforts have taken off in recent years. At the University of Kentucky, Dr. Lori Shook, Dr. Agatha Critchfield, and colleagues started the PATHways program in 2014 to support women during pregnancy and through the first five years of their babies’ lives with a wide variety of services, from domestic violence counseling and recovery groups to infant massage, acupressure, and aromatherapy. Prior to that, Critchfield said, “there was no viable place for women to go.”
Since the program started, the average length of stay in the NICU for NAS babies in the program has dropped from 29 days to six, and 97 percent of the babies kept with their mothers during treatment require no opioid medications.
At Yale New Haven Children’s Hospital, under the guidance of Dr. Matt Grossman, doctors in 2014 started using the “Eat, Sleep, Console” model, in which they put babies who had been exposed to opioids in utero in low-stimulation rooms with their parents sleeping in the hospital. Babies were comforted frequently, but only given morphine on select occasions. According to a study published in the journal Pediatrics last year, the percentage of infants being treated with morphine dropped from 98 percent to 14 percent, and the average stay decreased from 22 days to six.
Despite recent efforts at Yale and the University of Kentucky to move away from using medication with most babies, Magarian has stuck with his morphine protocol over the years. While he knows these other programs have gotten good results, he can’t quite shake his concern that the babies will suffer without more gradual weaning.
In 2014, Dominican Hospital closed its pediatric outpatient clinic and Magarian relocated to the East Cliff Family Health Center, a non-profit community clinic a few miles away, where he continues to see almost all of Santa Cruz’s drug-exposed infants. Magarian laments the loss of the set-up at Dominican in which he could confer with a multidisciplinary team on site, and he worries, in particular, about the loss of coordinated prenatal care. But he remains proud of Santa Cruz’s efforts.
Magarian expects the babies in his care to flourish, but he also knows how fragile they — and their mothers — can be. Lisa Castillo knows it, too. Speaking to Dr. Magarian about Jose at his checkup, she says, “He stays with me unless something goes sour.”
Still, she marvels at the opportunity to finally raise her own baby. Jose follows her voice now, she tells the doctor. He likes tummy time. Magarian suggests it is time to reduce Jose’s tiny dose of morphine to 0.2 milliliters. Then to 0.1 milliliters a few days later.
“And then you’re done,” he smiles.
Jocelyn Wiener is a freelance journalist based in Oakland, California. Her work has appeared in Kaiser Health News, The Atlantic, The Washington Post, and The Christian Science Monitor, among other outlets.