Covid Put Remote Abortion to the Test. Supporters Say It Passed.
Last summer, Cindy Adam and Lauren Dubey received the news they had hoped for, but hadn’t expected to get so soon. Their new telemedicine clinic would be able to offer remote medication abortion services, at least for the time being.
Medication abortion — which most commonly involves taking two medications, 24 to 48 hours apart, during the first 10 weeks of pregnancy — has been available in the U.S. since 2000. But, despite a growing chorus of advocates and experts who say remote access is just as safe as in-clinic care, the Food and Drug Administration requires providers to dispense mifepristone, the first of the two medications, inside the walls of a clinic, hospital, or medical office, citing the risk of complications. Most abortion providers interpreted this language to mean they could not mail mifepristone to patients’ homes, rendering fully remote abortion care impossible.
That changed in July 2020, when, due to the Covid-19 pandemic, a federal judge suspended the requirement, allowing remote abortion — also referred to as no-touch, no-contact, or direct-to-patient care.
Adam and Dubey, who are both nurse practitioners in California, took note. They launched medication abortion services in October 2020, as part of a telehealth clinic they called Choix. Within weeks, more than a dozen patients received medication abortions without having to leave their homes. “We hope to make it not this underground thing where you are getting medications from another country,” Dubey said in an interview last fall. “If that’s what it has to be, fine, but we want to be a mainstream source for being able to access medication pills by mail.”
Other providers raced to take advantage of the ruling, too. Just the Pill, which started seeing patients in October, offered telemedicine abortion services in Minnesota. Hey Jane launched in late 2020 with services for patients in Washington and New York.
It didn’t last long: On Jan. 12, the U.S. Supreme Court, in its first decision on abortion with Justice Amy Coney Barrett on the bench, struck down the lower court’s decision. Over a dissent from Justice Sonia Sotomayor, joined by Justice Elena Kagan, the Court’s majority argued that the lower court did not have the authority to lift the requirements of the FDA, “with its background, competence, and expertise to assess public health.” Choix suspended its medication abortion service. It was unclear if, when, or how they’d be able to offer it again.
“It definitely came as a big and devastating surprise,” Adam wrote in an email to Undark.
Their saga is the latest chapter in a long-running effort to expand the horizons of medication abortion — one that has run up against legal and regulatory hurdles for years in the United States.
Advocates say this window of time offered further evidence that fully remote abortion can work in the U.S., and that, for many patients, a visit to a physical clinic is unnecessary. Those claims draw on years of research, including data collected during the pandemic. But they’ve butted up against the objections of anti-abortion activists and the FDA policy that classes mifepristone as having “serious safety concerns,” leaving an uncertain future for this type of practice.
“For six months, medically-eligible patients were able to safely access medication abortion care through telemedicine and the mail,” Julia Kaye, a staff attorney at the American Civil Liberties Union (ACLU) Reproductive Freedom Project, wrote in an email to Undark.
“It is outrageous,” she added, “that abortion patients are once again being singled out for needless and arbitrary barriers to care.”
More than 600,000 people in the U.S. access abortion care each year. However, the ease of access varies significantly depending on a patient’s location and circumstances. Many have to travel long distances to clinics, especially in states with vocal anti-abortion movements. A majority of U.S. counties do not have an abortion clinic, and even in some cities, the nearest clinic may be more than 100 miles away.
The majority of early abortions in the U.S. are in-clinic procedures known as vacuum aspirations, which use suction to empty the uterus. But today, approximately 40 percent of abortions are induced with pills. The two-drug regimen consists of mifepristone, which blocks the hormone progesterone that is needed for a pregnancy to continue, and misoprostol, which causes contractions to push the pregnancy out.
Physicians and other experts, drawing on years of peer-reviewed research, say the combination of drugs do not typically require close, in-person medical supervision. When mifepristone was first approved by the FDA, abortion rights advocates like Elisa Wells hoped that it would ultimately improve access to abortion by moving it out of the realm of specialized abortion clinics and into common health care settings, like primary care and family medicine. Decades later, she said, that promise has yet to be fulfilled.
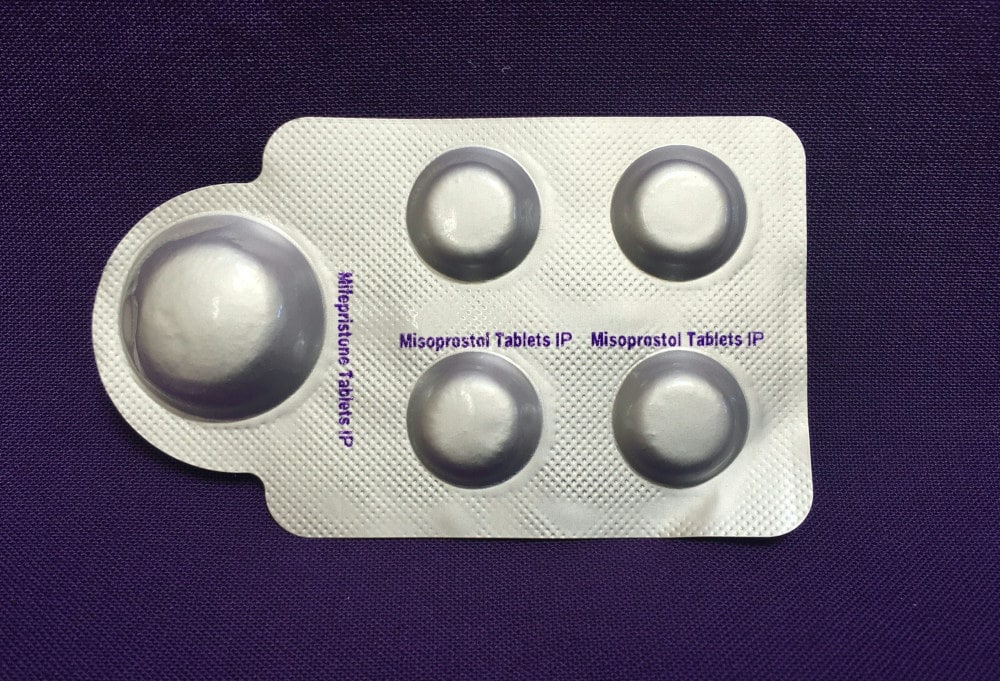
A combination pack of mifepristone and misoprostol tablets, which are used together to induce an abortion up to 10 weeks into pregnancy.
Visual: Elisa Wells / Plan C / AFP via Getty Images
“It’s already been 20 years since 2000,” said Wells, the co-founder and co-director of Plan C, a campaign that aims to raise awareness about medication abortion. “For 20 years, we’ve known the pills are safe and effective,” but “access is no better.”
The principal obstacle is the FDA, which classifies mifepristone under the agency’s Risk Evaluation and Mitigation Strategy (REMS) program. REMS is meant for drugs known to have serious safety concerns. Of the 20,000 prescription drugs approved by the FDA, just 60 fall under REMS, among them powerful antipsychotics and cancer drugs.
FDA documents explain that “the goal of the REMS for mifepristone is to mitigate the risk of serious complications.”
But those regulations have frustrated many physicians, who say they are motivated more by politics than patient safety. Jessica Beaman is a primary care physician in the San Francisco Bay area who also provides abortions. Because of the FDA regulations, Beaman cannot provide medication abortion as part of her primary clinic. She has to go to a separate practice, housed on a different floor of the same building, to prescribe the pills. Beaman said that she regularly prescribes other medications — for diabetes and heart disease, for example — that have far higher rates of complication than mifepristone.
Those drugs “are high risk and necessary for patients,” said Beaman, adding that she’s “able to stock those in my clinic without any kind of additional regulations.”
The disparity between the risks of medication abortion and the intensity of the regulations around it have led to repeated calls over the years from activists and major medical associations to remove the REMS. In 2016, the FDA revisited and revised the protocol. Patients still had to be given mifepristone within the confines of a clinic, but they could swallow the pill wherever they wanted. (The FDA declined to comment for this story, citing pending litigation over the REMS designation.)
Still, it remains challenging for many clinics to stock the drugs. And, experts say, the restrictions are one reason medication abortion costs, on average, more than $500.
“Because of the REMS, there’s just hoop, hoop, hoop, hoop, hoop, after hoop, and that just adds to the cost,” Wells said.
In 2017, Graham Chelius, a family medicine doctor in Hawaii, filed a lawsuit, with the help of the ACLU, challenging the FDA’s REMS restrictions. Chelius practices on the island of Kauai, which does not have an abortion clinic. Because the REMS prevents him from stocking and dispensing mifepristone onsite at his practice, Chelius has to turn those patients away. Anyone seeking an abortion on Kauai has to fly hundreds of miles round trip flight to another island to get the pills.
Lifting the REMS restrictions would lead to “a dramatic increase in access to abortion services,” Chelius told Undark.
The case was slowly making its way through the courts when the pandemic hit and a provisional window opened for a new kind of early abortion care.
Even knowing the window was likely to be temporary, some clinic leaders took note — including Adam and Dubey. The two met in 2012 while attending a nursing graduate program at the University of California, San Francisco. After graduating from UCSF, Adam stayed in the Bay Area, working for public health organizations. She also spent a couple years working for an online service for birth control pills, where, she said, she saw the positive impact that remote health care could have on people’s lives.
Dubey moved to Los Angeles after graduation and began working for Planned Parenthood, where she also began thinking about opportunities for telehealth. Many patients traveled long distances to get to her clinic, including from neighboring states, like Arizona, where abortion was more heavily restricted. “I would frequently see patients in the clinic waiting for medication abortion for hours at Planned Parenthood because we were so busy,” said Dubey. “Sometimes they’d have to leave to go pick up their kids from school.”
In 2019, the two began to discuss the idea of building an online clinic that provided sexual and reproductive health care via telemedicine. From the outset, they wanted to provide medication abortion, but they didn’t see a clear legal way.
By the summer of 2020, Choix’s platform was gearing up to launch without abortion services. Then the district court ruling came down, which said that the FDA must temporarily suspend the dispensing requirements during the pandemic. This meant abortion providers could now mail or arrange delivery of mifepristone to patients.
Adam and Dubey decided to move forward with a remote model. So did Julie Amaon, who came on as medical director at Just the Pill last summer to improve access to medication abortion in rural Minnesota. She was trying to figure out a way to offer no-touch abortions when the July ruling came down.
Kiki Freedman, founder and CEO of Hey Jane, also saw an opportunity. Freedman, who has a background in the technology industry, started working on Hey Jane in 2019, as a student at Harvard Business School. “We were interested in companies like Roman and Hims, that were advertising a ton at the time, and increasing access to stigmatized products for men,” she said, referring to successful startups that ship drugs for erectile dysfunction, hair loss, and other issues. “We thought, ‘Hey, this is a model that could be applied to the abortion world.’”
At Choix, Adam and Dubey moved quickly. With some financial and planning support from Plan C, they established a supply of mifepristone and found an online pharmacy partner. They then adapted the remote care flow they had developed for other services, like birth control pills and emergency contraception, to work for medication abortion.
To use the services, patients clicked through an “abortion care” button on Choix’s website. They signed a series of consent forms and filled out a health history questionnaire, which included questions to ensure they had access to medical care, such as a nearby emergency room, in the rare event of complications.
 |
For all of Undark’s coverage of the global Covid-19 pandemic, please visit our extensive coronavirus archive. |
Under most telemedicine abortion models, the patient and the health care provider participate in a secure video call. Instead, Choix offered an asynchronous approach: Patients sent in their information, and then Adam or Dubey reviewed the questionnaire. If they deemed the patient eligible for medication abortion, they sent the prescription to a digital pharmacy, which mailed the pills to the patient. Follow-ups happened through text messages, email, or phone. The whole process cost $199, with a sliding-scale payment option available for people unable to pay full cost.
Remote service does not work for all people seeking abortions, Dubey said. People who don’t have easy access to the internet, who don’t have stable housing, or whose homes lack safety or privacy may want or need to access in-clinic care, along with people who have certain medical conditions, such as a blood clotting disorder, that could lead to complications. Some patients simply prefer surgical abortions because they take less time to complete. However, advocates say, remote service has clear benefits, which Wells says boil down to “convenience, confidentiality, and control.”
Choix had provided medication abortion services to some 100 patients by Dec. 29, Adam wrote in an email at the time. Even though Choix does not ask patients about the circumstances that surround their decision to have an abortion, Adam said patients often volunteered that information and why the no-contact model worked for them.
“We heard stories from a patients who — one who has two children with disabilities and is currently managing at home during Covid without much support,” Adam said in November. “She said ‘I am so grateful I didn’t have to leave the house to do this. I can’t have another child.’ She was doing the best for her family right now.”
The push for remote medication abortion in the U.S. draws on research that stretches back more than a decade. In 2008, clinics in Iowa began offering telehealth abortion: Patients could go into a clinic and meet virtually with a doctor, who was at a different location. After the virtual visit and routine testing, supervised in-person by nurses or physician assistants, the doctor remotely unlocked a drawer that held the pills. The patient then took the mifepristone while the doctor watched on video conference, and later took the misoprostol pills at home.
Researchers analyzed data from the Iowa clinics about adverse events and outcomes, finding it was just as safe as in-person care. Data from the U.S. has been joined by studies from around the world reaching a similar conclusion. One systematic analysis published in May 2019 found that rates for surgical intervention after medication abortion were higher than expected. But the study noted this may reflect differences in local practices, and concluded that overall safety outcomes were similar between telemedicine and in-person care.
The studies did not include randomized clinical trials and most were based on self-reported outcomes. But researchers like Daniel Grossman, the lead author on the Iowa study, said that does not raise serious questions about safety.
Grossman, who directs the Advancing New Standards in Reproductive Health (ANSIRH) center at UCSF, has a career that has spanned advocacy and research, including stints as a researcher at Ibis Reproductive Health, a nonprofit with a mission to “advance sexual and reproductive autonomy, choices, and health worldwide,” and as a consultant to Planned Parenthood. Studies of clinical outcomes of telemedicine, he said, consistently “show that, not surprisingly, the effectiveness of the abortion is the same,” said Grossman. “In terms of the risks, we don’t see any evidence of an increased risk of complications.”
Despite such evidence, 19 states have laws that ban telemedicine abortion. In response, researchers have worked to gather more data to demonstrate the safety of remote models. In 2016, Gynuity Health Projects, a reproductive health research group supported by donors like the Bill and Melinda Gates Foundation, Planned Parenthood, and the Population Council, launched the TelAbortion Study, with approval from the FDA, to evaluate the use of medication abortion provided by telemedicine and mail. Patients participating in the study complete a video evaluation with a provider online, visit a nearby medical facility for routine tests like ultrasounds and bloodwork if needed, and then receive the pills in the mail to take at home. One of the objectives of the study was to demonstrate that mailing abortion medication was feasible and posed no additional risks.
“Every other aspect of the medical abortion did not require the patient to be physically present in the clinic, except the dispensing of the drug,” said Elizabeth Raymond, a senior medical associate at Gynuity. The organization started the study in 2016, she added, because the status quo “didn’t seem sensible.”
The TelAbortion study is now operational in 17 states and the District of Columbia and has served more than 1,700 patients. In a March article in the journal Contraception sharing some of the study’s findings, the researchers from Gynuity and other organizations concluded that the “direct-to-patient telemedicine service was safe, effective, and acceptable.” (Both Grossman and Raymond are members of the journal’s editorial board.)
The next frontier, advocates and experts say, is the one step of the medication abortion process that cannot be done from home — lab tests and ultrasounds. Typically, before administering mifepristone, physicians check to make sure the patient is not more than 10 weeks pregnant and does not have certain conditions, like an ectopic pregnancy or a bleeding disorder, that could lead to complications.
Over the past few years, research from Gynuity, along with Grossman’s team at UCSF and elsewhere, has suggested that all this testing may be unnecessary. Grossman said multiple studies have found that most women are able to accurately confirm their pregnancies with at-home tests and to date their pregnancies, based on their last menstrual period, with great accuracy. The World Health Organization, the American College of Obstetricians and Gynecologists, and peer organizations in the U.K. and elsewhere have concluded that ultrasounds to rule out ectopic pregnancy are unnecessary in people without risk factors or symptoms.
Based on this data, Grossman, Raymond, and others put together what is known as the “no-test protocol,” in which eligible patients can forego pre-abortion testing and are screened primarily based on their medical history.
“All the information we have so far certainly indicates that it’s safe and safe enough for providers to be using right now,” Grossman said of the protocol.
Research into the no-test protocol was underway before the pandemic hit. Women on Web, a nonprofit founded in 2005, has mailed abortion pills to tens of thousands of patients around the world, primarily in countries where abortion is illegal. (The organization also runs a U.S. program, called Aid Access, which has sent abortion pills to thousands of patients through unofficial channels). By necessity, the model is fully remote, and Women on Web staff only screen women by their self-reported medical history. “No serious adverse events were reported that resulted from the omission of the tests,” Raymond and Grossman, along with a group of other experts and advocates recently wrote in a commentary in the journal Contraception, reporting on the data. (Two authors of the paper are consultants for companies that manufacture mifepristone.)
During the pandemic, more providers have adopted the protocol. “The medical community is getting on board with a no-test protocol,” said Wells, of Plan C. “ACOG, the Royal College in the U.K. — everybody changed the standard of care overnight.”
Some physicians have pushed back against adoption of the no-test protocol. The Charlotte Lozier Institute, which serves as the education and research arm of Susan B. Anthony List, a nonprofit dedicated to ending abortion in the U.S. by supporting anti-abortion politicians, published a paper in July referring to the approach as “cavalier.” The paper was written by Ingrid Skop, a member of the board of the American Association of Pro-life Obstetricians and Gynecologists. In the paper, Skop wrote that the studies used by groups like ACOG to show the safety of the no-test protocol are based on biased data and under-reported complication and efficacy rates that make medication abortion seem less risky than she believes it is. (Emails to the Charlotte Lozier Institute and Susan B. Anthony List about the research went unanswered.)
Grossman contests their finding. He also said there’s little evidence that a raft of pre-abortion testing leads to improved safety. “I do agree that it will be important to collect data on how the protocol works in practice and document clinical outcomes,” he said. “Maybe aspects of the protocol will need to be tweaked or clarified to better identify the patients who would be best served by an ultrasound, but all the information we have so far certainly indicates that it’s safe and safe enough for providers to be using right now.”
Choix, Just the Pill, and Hey Jane each adopted the no-test protocol as part of their services for patients who knew the date of their last menstrual period and showed no signs of contraindications. If patients cannot date their last period, Choix will refer them to get ultrasounds before proceeding with the process.
“This is a completely new model of care that we’re doing,” said Adam during a conversation last fall. “We have to be very careful with patients’ health and safety and require an ultrasound if they are not positive of their period date, or if there are other factors.”
The Supreme Court decision in January did not address these scientific questions, instead deferring to the authority of the FDA. In a 12-page dissent Justice Sonia Sotomayor challenged the FDA’s policy. She asked why the agency had waived in-person requirements for certain prescription drugs, including opioids, due to concerns about Covid-19, but has “refused to extend that same grace to women seeking medication abortions.” And, in the six months since the in-person requirements were suspended, she wrote, “the government has not identified a single harm experienced by women who have obtained mifepristone by mail or delivery.”
Despite the Supreme Court shutdown, advocates say the brief window of remote abortion has helped raise interest in the practice among traditional abortion providers. “The genie is out of the bottle,” said Wells. Over the past few months, Plan C has helped organize webinars about how to offer remote abortion care that have attracted hundreds of participants from across the country.
“This is the future,” Wells said. “It’s perfect during a pandemic, and it’s perfect not during a pandemic.”
Following the Supreme Court’s decision, Choix halted its medication abortion service, though Adam and Dubey say the clinic has recently begun providing mifepristone in the office. They continue to mail misoprostol. At Just The Pill, Amaon and her team reverted to their original plan and are currently delivering pills with a mobile clinic. Hey Jane, after temporarily suspending services, decided to continue operating their pills-by-mail service for eligible patients, testing a novel legal interpretation of the REMS. The interpretation, which hinges on a specific definition of the word “dispense,” is yet to be tested in court.
“The patient need right now is so salient and urgent that it wouldn’t be right for us to continue to shut down,” Freedman said.
Advocates are also calling on President Joe Biden’s administration to lift the in-person dispensing requirement for the duration of the pandemic and to direct the FDA to review the REMS for mifepristone, geared towards more permanent change. In early February, they were joined by a group of House Democrats, who asked the FDA to “immediately eliminate the medically unnecessary in-person dispensing requirement for mifepristone” in a letter.
“We absolutely think that the impact will be more long-lasting,” Adam wrote in an email, “and that this has helped move the frontier of what is possible with abortion access forward.”
Rebecca Grant is a freelance journalist based in Portland, Oregon, who covers reproductive rights, health, and justice.











