A Mobile Health Clinic Is Bringing Contraception to the Rio Grande Valley
In early 2016, Joseph Potter traveled to the Rio Grande Valley to discuss worrisome findings about contraception access in Texas. As a professor of sociology at the University of Texas at Austin, Potter had long studied women’s access to contraception during the initial months after childbirth. This is a time when women, particularly those covered by Medicaid, are most likely to get regular health care. “It’s also a time,” said Potter, “when the vast majority of women do not want to get pregnant again.”
In his study of eight Texas hospitals, Potter had found that slightly more than three-fourths of 1,700 new mothers — virtually all of them on public insurance — indicated interest in using the most effective form of contraception, either sterilization or a long-acting reversible device, such as an implant or an intrauterine device (IUD). But six months later, nearly half of these women were relying upon something else, including vulnerable methods such as condoms or withdrawal.
Roughly half an hour from the Mexican border, in the city of Edinburg, Potter met with Aida Gonzalez, vice president of DHR Health Women’s Hospital. They were joined by Tony Ogburn, chair of the Department of Obstetrics and Gynecology at the University of Texas Rio Grande Valley School of Medicine, then a brand new medical school that was about to welcome its first class. Ogburn was eager to improve women’s health care in the underserved border region, and Potter’s data, which included responses from women who had delivered at Women’s Hospital, offered a starting point. Among the other findings: just 10 percent of new mothers at Women’s Hospital were discharged after delivery with some form of contraception versus 23 percent across the eight hospitals studied.
Ogburn and his colleagues believed local women needed better access, including to the costlier and most reliable devices: IUDs and implants. By cobbling together several grants, and teaming up with Women’s Hospital, they’ve so far been able to provide the devices at little to no cost through the medical school’s outpatient obstetrics/gynecology clinic, a mobile outreach effort, and at the hospital immediately after delivery.
Long-acting reversible contraception, frequently dubbed LARC (pronounced “lark”), is strikingly effective at preventing unwanted pregnancies, and studies suggest its failure rate is a mere fraction of other methods, including the pill. And yet in 2017, only about 11 percent of women nationwide made use of long-acting reversible contraception for various reasons, including lack of insurance coverage or inadequate training on the part of their health provider. But for low-income women, the price tag is an even bigger barrier; the devices alone cost roughly $750, according to Ogburn. The high cost also discourages hospitals or doctors in private practice from keeping many, or sometimes any, in stock.

A decade-long effort by women’s health advocates has sought to improve access to the full spectrum of birth control methods, and especially LARC. But reproductive justice activists argue and some physicians acknowledge that such outreach efforts, no matter how well-intentioned, carry the risk of becoming coercive if clinicians impose their own family planning values on patients, particularly those who are lower-income or people of color.
That was one of Gonzalez’s first concerns when another OB/GYN at the medical school approached her later that year about launching a program to offer LARC immediately after delivery, before going home. Sitting in her first-floor office, just down the hallway from the hospital’s nursery, Gonzalez said that any post-delivery program should be designed in such a way that women were educated in their options and wouldn’t feel pressured to choose LARC, or even any contraception.
“I was wanting to make sure,” she said, “that it wasn’t gonna portray that our hospital was targeting low-income Hispanic women.”
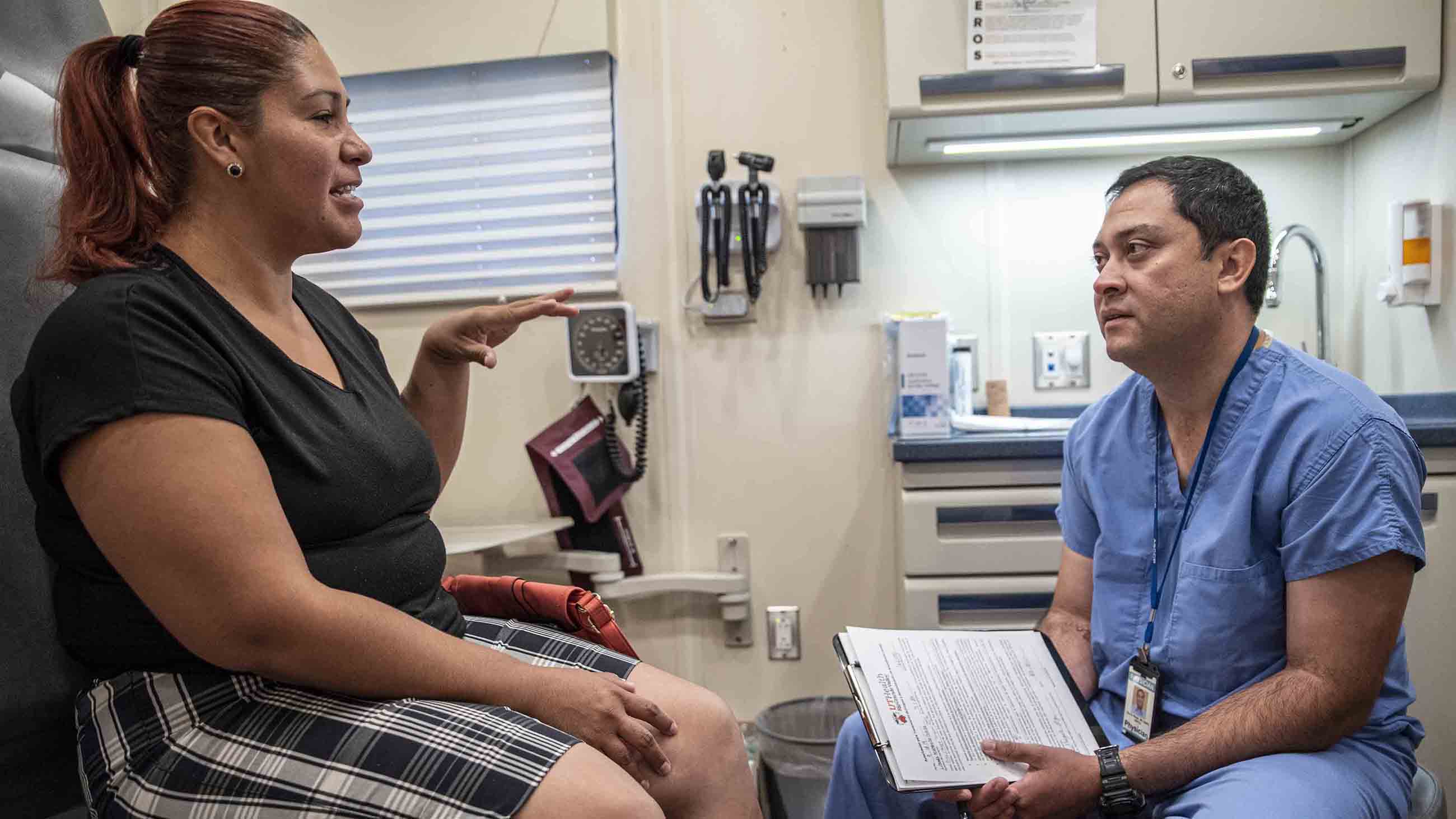
The University of Texas Rio Grande Valley’s 40-foot-long mobile clinic is a tight fit with an exam room at either end, a tiny bathroom used as a storage closet, and sometimes as many as eight people inside, including Saul Rivas, the lead physician, a nurse practitioner, a physician resident, a medical school student, a medical assistant, and perhaps another health worker and one or two patients. On a recent summer day, most of the women who climbed the steep metal stairs into the clinic, dubbed the Unimóvil, had already gotten contraception counseling elsewhere, through the medical school’s outpatient clinic or from one of the community health workers — promotores — who work with the LARC program.
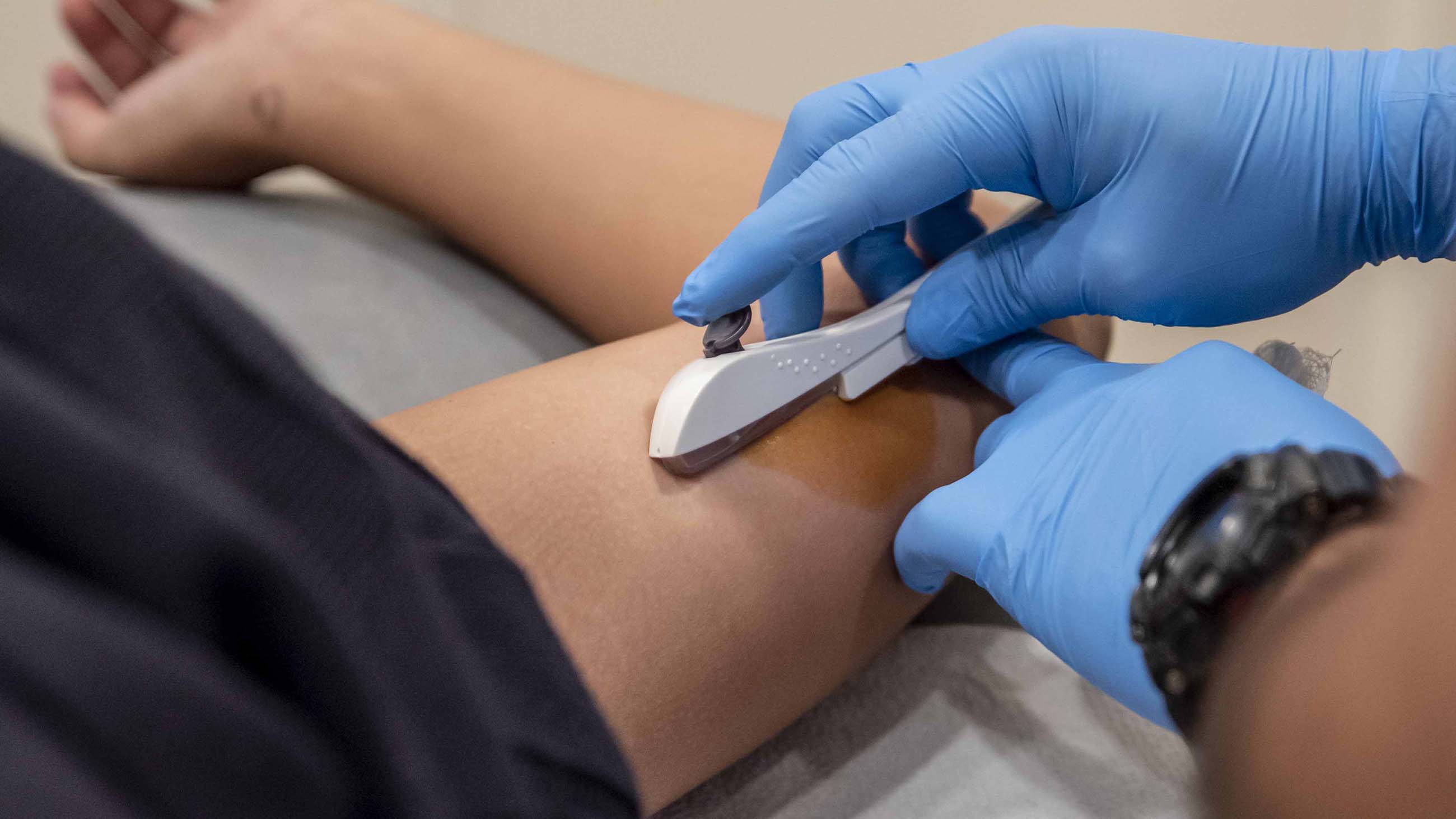
A linchpin of the medical school’s LARC commitment, the clinic has been visiting isolated lower-income communities once a month, most months, since early 2018. Long-acting reversible contraception — reversible because women can get pregnant shortly after the device is removed — includes two types. The implant, often described as a matchstick-thin rod, is inserted just under the skin of the upper arm. The IUD, a tiny flexible T-shaped device, is inserted into the uterus.
This was the clinic’s second visit to Penitas, a rural community of nearly 5,000 residents located by the banks of the Rio Grande river. Lizeth Avila, one of the day’s first patients, lived so close that she could see the clinic from her home. The 24-year-old mother of three had previously used an IUD. But since Avila’s daughter was born last fall, she and her husband had relied first on the Depo-Provera shot and more recently on condoms. Her husband was interested in having another child, Avila told clinicians, but she felt differently. Her pregnancies had been difficult, with a form of extreme morning sickness that caused near-constant vomiting. “I had it with them three [pregnancies],” she said. “But my latest one, I actually did go to the hospital for a week.”
Avila listened closely as a physician resident asked about her prior and current contraceptive use, along with her preferences. From the start, Avila was pretty sure that she wanted the same non-hormonal IUD she’d used previously. (She returned for the procedure later that day, when the clinic had the IUD in stock.)
Shortly afterward, another woman, Tania Rodriguez, was escorted into one of the exam rooms. She was there to replace her existing implant before it became ineffective. After giving birth to two children before the age of 18, the 23-year-old said that she didn’t want to take any chances.
Rodriguez was given an injection to numb the area on her upper arm, then Rivas verbally guided the physician resident through the removal of the existing device, which had been inserted by clinicians practicing elsewhere. “It’s a little bit deep, but I think that we can get it out,” Rivas said.
Rodriguez kept her head turned away to the side, preferring not to look. “Ok, just grab the tip,” Rivas told the physician resident.
By day’s end, more than a dozen women walked in for appointments and all but one left with an IUD or an implant. More women were trying to get in and one promotora’s phones continued to vibrate with calls and texts from women checking to see if a last-minute cancellation had opened up a slot.
This stretch of the Texas-Mexico border, which includes the two most populous counties in the Rio Grande Valley, Cameron and Hidalgo, is dominated by private practices and for-profit hospitals. (Women’s Hospital, a free-standing facility, is part of physician-owned DHR Health.) There’s no public hospital in either county. Nearly one-third of the 1.3 million residents are uninsured versus 8.5 percent nationally. Nine out of 10 residents are Hispanic, and the median household income is roughly $37,000.
In 2016, pregnancy rates in the Rio Grande Valley, among teens ages 15 to 19 years old, ran more than twice the national average, with 4.4 percent to 6.9 percent becoming mothers compared with 2 percent among teens nationally, according to an analysis of state data by the Texas Campaign to Prevent Teen Pregnancy.
But unplanned pregnancies at any age are far from rare. Nearly half of all pregnancies in the U.S. are either poorly timed or unwanted. Offering reliable contraception to women “opens up the world,” Ogburn said. “Being able to have the opportunity to say, ‘I don’t want to be pregnant now, I want to keep working.’ Or ‘I want to go to school,’ or ‘I want to stay home and take care of the kids that I have,’” he said. “It’s a game changer.”
Still, clinicians must guard against their own biases when counseling patients about options, cautioned Jamila Taylor, now the director of health care reform and a senior fellow at The Century Foundation, a 100-year-old progressive think tank. “OB/GYNs can be of the mindset that, ‘This woman is vulnerable,’” Taylor said. “‘She’s low income. She can’t afford to have another pregnancy any time soon. This is for her own good to have a long-acting contraceptive method.’”
Sometimes, far more egregious examples of coercion hit the headlines. In 2017, an order issued by a Tennessee judge to reduce female inmates’ sentences by 30 days if they agreed to get an implant, was rescinded after media coverage and related criticism.
Potter acknowledged that there’s always a risk that over-zealous clinicians can lobby patients to choose LARC. “But if that exists in Texas, it’s a teeny, teeny fraction,” he said. “A much larger more prevalent problem is people not having access to the LARC that they’d like to have.”
Nationally, 11.3 percent of women have chosen long-acting reversible contraception in recent years — a small percentage overall, but a marked uptick over the last decade, and one driven in part by the backing of the American College of Obstetricians and Gynecologists (ACOG). In 2015, the physicians’ group released a committee opinion advising that more women should be encouraged to consider an implant or IUD. Also many states, including Texas, now cover LARC through their Medicaid program if clinicians place the device immediately after delivery.

LARC proponents will point out that you can’t “forget to use” an IUD or an implant. Thus in real-world experience, the devices are far more effective than even the birth control pill, with failure rates ranging from 0.3 percent to 0.9 percent, according to a large-scale study which tracked three years of pregnancies in 7,486 women. The failure rate for the birth control pill, which was studied as a group along with the patch and the vaginal ring, ranged from 4.8 percent to 9.4 percent for those same three years, researchers reported in 2012 in the New England Journal of Medicine. (The pill is 99 percent effective if taken every single day without fail.)
Eve Espey, a New Mexico obstetrician/gynecologist and a long-term LARC proponent, said that some compelling and appropriate criticism did flare in the wake of that 2012 study’s publication. The participants were able to choose their method but were provided a contraception chart that critics maintained had placed disproportionate emphasis on effectiveness, by ranking them that way, she said. Some women might have other priorities, reproductive justice advocates pointed out, such as avoiding specific side effects or being able to go off birth control without a clinician’s assistance.
“It was felt like the script was somewhat coercive,” said Espey, who chairs the American College of Obstetricians and Gynecologists’ LARC working group and helped write the 2015 opinion. The language in that opinion, which recommended that physicians “encourage consideration of implants and IUDS for all appropriate candidates,” will be revisited and likely softened, including its emphasis on reducing unintended pregnancy, Espey said.
“The whole concept of unintended pregnancy is really drawing a lot of criticism right now,” Espey said, “because it implies that that’s always a bad thing and it also implies that we may value pregnancies in some populations more than we value those in others.”
Ogburn made a similar point in the context of the teen pregnancy rate, which he said has been typically tracked because having a baby at that young age has been viewed negatively. “It’s looked at as a failure of the system,” he said. “That they either shouldn’t be having sex, or if they do have sex, they should have birth control.” But Ogburn also recalled teen deliveries, when he worked years ago in the Indian Health Service, that were a celebratory event, with several generations in attendance.
Ogburn and Rivas, who co-lead the medical school’s LARC outreach, said that they’ve strived to prevent even subtle coercion by providing patients information on all options and, during prenatal visits, starting as early in the pregnancy as possible. Plus, the medical school has made a commitment — one that they’ve been able to fulfill with the help of a grant from a private donor — to get LARC to anyone who wants it. Moreover, the school will provide follow-up care, including removing the device if the woman decides she doesn’t like it or wants to get pregnant.
Still, ensuring clinicians don’t unconsciously frame or steer discussions toward LARC remains a constant battle, said Ogburn. “Because we all do have implicit bias.”
For instance, Ogburn described one of the physician residents as a warm-hearted doctor, but also a bit of a “zealot” regarding the devices. She had expressed concern that a recent patient planned to continue relying on condoms after delivery. Ogburn countered that the woman, who was in her late 30s and had just delivered her second child, seemed comfortable with her approach. “Her and her husband have figured out what works for them,” he said.
Until recently, easier LARC access in the Rio Grande Valley has been hindered by gaps in clinician training, along with challenges related to cost and reimbursement, said Rivas, who grew up in El Paso. Driving down a quiet road early one morning in his aging truck, en route to meet up with the Unimóvil in Penitas, Rivas started ticking off the various obstacles – including the high cost and the fact that many doctors and clinics simply don’t stock the contraceptives.
If a woman prefers to get an IUD or an implant, Rivas said, she’ll likely have to return for a second visit, difficult for any busy woman and more so for a new mom struggling to make ends meet. “Those folks tend to have to return to work sooner usually or they have more kids they’re taking care of at home,” he said. “They already have transportation issues. They already have [health care] access issues.”
As part of its post-delivery LARC program with the medical school, Women’s Hospital has been keeping the devices in stock. And there’s been demand. Over a span of two and a half years, 332 IUDs and implants were provided to women through the program, 296 immediately after delivery, according to the medical school.

Slightly more than two-thirds of the devices have been paid for through a private grant by an anonymous donor. For the remainder, the hospital has pursued reimbursement through insurance, primarily Medicaid. Initially reimbursement was a headache for several reasons, including that Medicaid managed care plans were not accustomed to being billed for this type of contraception. Ogburn and Rivas credit the Women’s Hospital staff with sorting this out in order to establish the program, which they describe as a rarity among non-public hospitals in Texas.
Meanwhile, the medical school has jump-started training, not only by teaching its physician residents to insert the devices, but also local nurse practitioners and other clinicians. To provide the implant, physicians and other clinicians must first complete a training course sponsored through Merck, the manufacturer.
When Ogburn — already a certified trainer who could teach others — arrived in the valley in 2015, he didn’t know of any other certified trainers. But since then, more than 100 clinicians have been trained in the four-county region, according to data that Ogburn provided from Merck.
Shortly before 7 a.m., the physician residents gathered in a conference room at Women’s Hospital, along with a few medical students and teaching faculty, to run through the shift hand off. They briefly reviewed the cases of women in the hospital, who was scheduled for surgery, who had delivered and their contraception plans.
To a large degree, the residents comprise the backbone of contraception education, informing patients of their options when they seek care at the medical school’s outpatient clinic and at Women’s Hospital. And bias can cut more than one way, said Rivas, describing rounding with the residents shortly after joining the medical school. A resident, who had been presenting a patient’s case, hadn’t mentioned the woman’s contraception preferences. So Rivas asked.
Her response, as he recalled the exchange: “‘Dr. Rivas, we really don’t talk about that stuff much over here, because these patients, they’re Hispanic and they’re Catholic.’” Rivas wryly pointed out that he carried one of those two attributes. “And I’ve talked to plenty of patients that are both of those two. And you can still have a discussion — at least find out, right?”
Now counseling has become routine, said physician resident Nazanin Ahmadieh, who stayed behind after the shift handoff with Denise De Los Santos, part of the school’s teaching faculty, to discuss their approach. It’s not uncommon, they said, for patients to not realize that there are alternatives to the birth control pill or the Depo-Provera hormonal shot.

Still energetic after an overnight shift, Ahmadieh gestured toward the two models of IUDs that hang from her work badge. That way, she said, she can easily demonstrate that the devices are smaller and more flexible than women might realize.
Along with checking on their patients’ future childbearing plans, Ahmadieh and De Los Santos ask other questions to help women figure out which method might work best for them. Do they travel a lot? Do they dislike injections? Can they remember to take a daily medication, such as a multi-vitamin?
They also provide a chart that ranks the effectiveness of various types of birth control with no emphasis, De Los Santos noted, on the underlying cost. It’s similar, she said, to how car dealerships position their most expensive models with the high-end safety and other features at the front of the show room. “I’m not going to tell you about the one that doesn’t work the best, first,” she said. “I’m going to tell you about the best one.”
Nidia Rodriguez was just several months pregnant, scarcely through her first trimester, when Ahmadieh first asked her and her husband, Gabriel, about whether they’d thought about what contraception they’d be using after delivery.
Rodriguez, now age 28, had become a mother early, giving birth to her first child as a teenager. Since then, she’d relied on various methods through the years, most recently the Depo-Provera shot, though she disliked what she described as painful injections. She isn’t a fan of birth control pills and the pressure to remember to take a medication every day.
But reliability mattered to her a lot. In fact, for years Rodriguez had been happy with one child.
“I didn’t think I was going to have another child, but he convinced me,” she said, smiling at Gabriel, whom she married in 2015. As Rodriguez talked, curled up on a sofa in her apartment, her 9-week-old daughter Emi cuddled closely against her chest, sucking on a pacifier.
Rodriguez, convinced that this baby would be her last, asked Ahmadieh about getting a tubal ligation. “But I guess because of my age she was like, ‘Oh, you might want to have kids later on.’”
Ahmadieh suggested an implant or IUD as an alternative, answering the couple’s questions about any risks, and then following up periodically during later appointments. It helped, Gabriel said, that they could check out the IUD models hanging from Ahmadieh’s badge, to see that it “was just that little thing.”
For Nidia and Gabriel, who over a series of prenatal visits settled on an IUD, getting the contraception was practically a non-event. Shortly after delivering her daughter and the placenta, the IUD was inserted, she said, and with it protection that lasts for five years — unless she decides to get pregnant again.
Charlotte Huff is a Texas-based journalist who writes about the intersection of medicine, money, and ethics. Her work has appeared in Kaiser Health News, Slate, STAT, and Texas Monthly, among other publications.