What You Should Know About Yellow Fever
Last week, the World Health Organization declared the yellow fever outbreaks in the neighboring African nations of Angola and the Democratic Republic of the Congo a “serious public health event,” but concluded that they did not constitute a Public Health Emergency of International Concern (PHEIC).
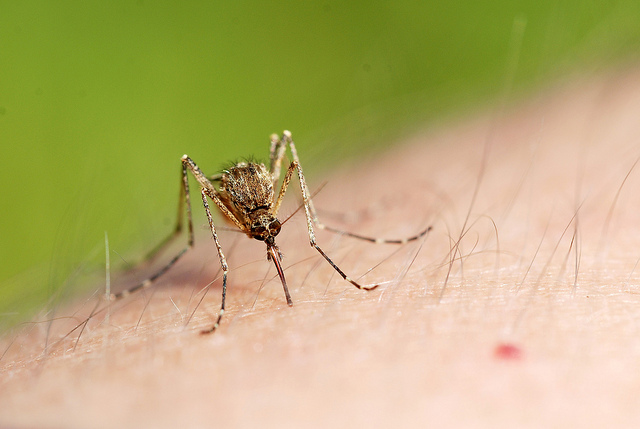
The same mosquitoes that spread the Zika and West Nile viruses are also spreading yellow fever. (Photo by Gilles San Martin/Flickr)
Under the WHO’s International Health Regulations of 2005, a PHEIC is defined as “an extraordinary event which is determined to constitute a public health risk to other States through the international spread of disease and to potentially require a coordinated international response.” The organization has only made this declaration four times: for Swine Flu in 2009, polio and Ebola in 2014, and most recently for the cases of microcephaly and Guillain-Barré Syndrome being caused by the Zika virus.
The recent yellow fever outbreak was first detected in Angola last December and is suspected to have infected over 2,400 people — of those, about 300 have died so far. While this number is so far small compared to other disease outbreaks, the WHO notes that it appears to be accelerating: cases increased 33 percent in the past five weeks. With vaccines in short supply, scientists worry that there is potential for the virus to spread and become a greater hazard.
Already, the Angola outbreak has spread as far as China and a separate, apparently unrelated outbreak began in Uganda this month. The Aedes aegypti mosquito — the same species responsible for Zika and West Nile virus — is the main vector for yellow fever and unfortunately, it can be found on every continent except Antarctica.
“The potential for it to cause many more infections and many more deaths and to spread to other countries and other cities is quite high,” said Daniel Lucey, an infectious disease researcher and Senior Scholar at the O’Neill Institute for Global Health Law at Georgetown University. “We’re looking at a cross section, a snapshot in time — a moment in time — and in my opinion it’s really important…to look forward to try and anticipate the trajectory of these two yellow fever epidemics.”
Lucey doesn’t think an outbreak in the U.S. is likely, but still says yellow fever is something that Americans — most of who are not vaccinated — should be aware of.
Historically the disease has remained mainly in Sub-Saharan Africa, but the U.S. — notably in the Southeastern region — experienced outbreaks up until the early 20th century. And around the world, yellow fever still kills 30,000 to 60,000 people every year. East Asia has never experienced an outbreak before, leading to concern that a lack of immunity there could exacerbate the situation.
Although the majority of people who do get yellow fever experience little-to-no symptoms, 15 percent become ill, suffering shock, dangerously high fevers and liver failure. Named for the color a person’s skin turns when liver damage sets in, yellow fever is fatal in about 15 percent of cases.
One strategy to deal with the limited vaccines is to split up the existing supply. Most people still gain some protection from yellow fever with just a partial vaccination. “Imagine if there’s another big city somewhere, so Windhoek or Lusaka or, heaven forbid, Lagos, or any city in Asia,” said Lucey. “Then we’re not going to have enough vaccine so were going to have to do this contingency plan of using maybe one-fifth of the normal dose.”
Such a strategy isn’t ideal, but it may be necessary. Yellow fever vaccines are still made using a slow, outdated technique: injecting the virus into fertilized chicken eggs. It’s a technique that Thomas Yuill, professor emeritus in the department of pathobiological sciences at the University of Wisconsin-Madison, refers to as an “arcane, wing-of-bat, eye-of-newt method.”
“That is where many, including myself, think that some serious emphasis need to be put,” said Yuill
There are currently only four facilities in the world that make the vaccine for yellow fever. While early attempts to create it in a new, faster way seem to have been successful, ramping up the production and making sure that the vaccine is safe could take months or years, said Yuill — and that’s if everything goes well. Until then, the WHO and infected countries will have to do make do with what vaccines they have.
According to Science, the WHO used up their emergency stockpile of vaccines earlier this year in Angola, but expects to have 7 million more by the end of the month. That’s a definite improvement but not, obviously, a solution to a major outbreak, for instance in a country like China, which has over 1 billion people and is home to densley-packed megacities like Shanghai and Beijing.
At the moment, “We have the capacity to make millions more vaccines, but not hundreds of millions,” said Lucey.
Still, for now, the outbreak seems to be under control and is definitely being closely monitored. Even Lucey, who has been critical of the WHO’s efforts to combat Zika and Ebola in the past, said that with yellow fever, the organization seems to be taking the right steps.
Correction: This post has been updated to correct a quote from Daniel Lucey. In listing cities where it would be dangerous to have a yellow fever outbreak, he said Lusaka, not Osaka.










